Cefdinir
CEFDINIR CAPSULES USP
FULL PRESCRIBING INFORMATION: CONTENTS*
- CEFDINIR DESCRIPTION
- CLINICAL PHARMACOLOGY
- CEFDINIR INDICATIONS AND USAGE
- CEFDINIR CONTRAINDICATIONS
- WARNINGS
- PRECAUTIONS
- OVERDOSAGE
- CEFDINIR DOSAGE AND ADMINISTRATION
- HOW SUPPLIED
- CLINICAL STUDIES
- REFERENCES
- PRINCIPAL DISPLAY PANEL
FULL PRESCRIBING INFORMATION
300 mg
Rx only
To reduce the development of drug-resistant bacteria and maintain the effectiveness of cefdinir capsules and other antibacterial drugs, cefdinir capsules should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.
CEFDINIR DESCRIPTION
Cefdinir capsules contains the active ingredient cefdinir, an extended-spectrum, semisynthetic cephalosporin, for oral administration. Chemically, cefdinir is [6R-[6α,7β(Z)]]-7-[[(2-amino-4 thiazolyl) (hydroxyimino) acetyl]amino]-3-ethenyl-8-oxo-5-thia-1-azabicyclo[4.2.0]oct-2-ene-2-carboxylic acid. Cefdinir is a white to slightly brownish-yellow solid. It is slightly soluble in dilute hydrochloric acid and sparingly soluble in 0.1 M pH 7.0 phosphate buffer. The molecular formula is C14H13N5O5S2 and the molecular weight is 395.42. Cefdinir has the structural formula shown below:
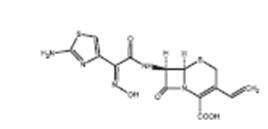
Cefdinir capsules contain 300 mg of cefdinir and the following inactive ingredients: carboxymethylcellulose calcium; colloidal silicon dioxide; and magnesium stearate. The capsule shells contain D&C Red #28; FD&C Blue #1; FD&C Red #40; gelatin and titanium dioxide.
CLINICAL PHARMACOLOGY
Pharmacokinetics and Drug Metabolism:
Microbiology:
As with other cephalosporins, bactericidal activity of cefdinir results from inhibition of cell wall synthesis. Cefdinir is stable in the presence of some, but not all, β-lactamase enzymes. As a result, many organisms resistant to penicillins and some cephalosporins are susceptible to cefdinir.
Cefdinir has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in INDICATIONS AND USAGE.
CEFDINIR INDICATIONS AND USAGE
To reduce the development of drug-resistant bacteria and maintain the effectiveness of cefdinir capsules and other antibacterial drugs, cefdinir capsules should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Cefdinir capsules are indicated for the treatment of patients with mild to moderate infections caused by susceptible strains of the designated microorganisms in the conditions listed below.
Adults and Adolescents:
Pediatric Patients:
CEFDINIR CONTRAINDICATIONS
Cefdinir is contraindicated in patients with known allergy to the cephalosporin class of antibiotics.
WARNINGS
BEFORE THERAPY WITH CEFDINIR IS INSTITUTED, CAREFUL INQUIRY SHOULD BE MADE TO DETERMINE WHETHER THE PATIENT HAS HAD PREVIOUS HYPERSENSITIVITY REACTIONS TO CEFDINIR, OTHER CEPHALOSPORINS, PENICILLINS, OR OTHER DRUGS. IF CEFDINIR IS TO BE GIVEN TO PENICILLIN-SENSITIVE PATIENTS, CAUTION SHOULD BE EXERCISED BECAUSE CROSS-HYPERSENSITIVITY AMONG β-LACTAM ANTIBIOTICS HAS BEEN CLEARLY DOCUMENTED AND MAY OCCUR IN UP TO 10% OF PATIENTS WITH A HISTORY OF PENICILLIN ALLERGY. IF AN ALLERGIC REACTION TO CEFDINIR OCCURS, THE DRUG SHOULD BE DISCONTINUED. SERIOUS ACUTE HYPERSENSITIVITY REACTIONS MAY REQUIRE TREATMENT WITH EPINEPHRINE AND OTHER EMERGENCY MEASURES, INCLUDING OXYGEN, INTRAVENOUS FLUIDS, INTRAVENOUS ANTIHISTAMINES, CORTICOSTEROIDS, PRESSOR AMINES, AND AIRWAY MANAGEMENT, AS CLINICALLY INDICATED.
Clostridium difficile associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including Cefdinir, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated.
PRECAUTIONS
General:
Prescribing cefdinir capsules in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug resistant bacteria.
As with other broad-spectrum antibiotics, prolonged treatment may result in the possible emergence and overgrowth of resistant organisms. Careful observation of the patient is essential. If superinfection occurs during therapy, appropriate alternative therapy should be administered.
Cefdinir, as with other broad-spectrum antimicrobials (antibiotics), should be prescribed with caution in individuals with a history of colitis.
In patients with transient or persistent renal insufficiency (creatinine clearance <30 mL/min), the total daily dose of cefdinir should be reduced because high and prolonged plasma concentrations of cefdinir can result following recommended doses (see DOSAGE AND ADMINISTRATION).
Information for Patients:
Patients should be counseled that antibacterial drugs including cefdinir capsules should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When cefdinir capsules is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by cefdinir capsules or other antibacterial drugs in the future.
Antacids containing magnesium or aluminum interfere with the absorption of cefdinir. If this type of antacid is required during cefdinir therapy, cefdinir should be taken at least 2 hours before or after the antacid.
Iron supplements, including multivitamins that contain iron, interfere with the absorption of cefdinir. If iron supplements are required during cefdinir therapy, cefdinir should be taken at least 2 hours before or after the supplement.
Diarrhea is a common problem caused by antibiotics which usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibiotic. If this occurs, patients should contact their physician as soon as possible.
Drug Interactions:
Drug/Laboratory Test Interactions
A false-positive reaction for ketones in the urine may occur with tests using nitroprusside, but not with those using nitroferricyanide. The administration of cefdinir may result in a false-positive reaction for glucose in urine using Clinitest®, Benedict’s solution, or Fehling’s solution. It is recommended that glucose tests based on enzymatic glucose oxidase reactions (such as Clinistix® or Tes-Tape®) be used. Cephalosporins are known to occasionally induce a positive direct Coombs’ test.
Carcinogenesis, Mutagenesis, Impairment of Fertility:
The carcinogenic potential of cefdinir has not been evaluated. No mutagenic effects were seen in the bacterial reverse mutation assay (Ames) or point mutation assay at the hypoxanthine-guanine phosphoribosyltransferase locus (HGPRT) in V79 Chinese hamster lung cells. No clastogenic effects were observed in vitro in the structural chromosome aberration assay in V79 Chinese hamster lung cells or in vivo in the micronucleus assay in mouse bone marrow. In rats, fertility and reproductive performance were not affected by cefdinir at oral doses up to 1000 mg/kg/day (70 times the human dose based on mg/kg/day, 11 times based on mg/m2/day).
Pregnancy:
Teratogenic Effects: Pregnancy Category B.
Cefdinir was not teratogenic in rats at oral doses up to 1000 mg/kg/day (70 times the human dose based on mg/kg/day, 11 times based on mg/m2/day) or in rabbits at oral doses up to 10 mg/kg/day (0.7 times the human dose based on mg/kg/day, 0.23 times based on mg/m2/day). Maternal toxicity (decreased body weight gain) was observed in rabbits at the maximum tolerated dose of 10 mg/kg/day without adverse effects on offspring. Decreased body weight occurred in rat fetuses at ≥100 mg/kg/day, and in rat offspring at ≥32 mg/kg/day. No effects were observed on maternal reproductive parameters or offspring survival, development, behavior, or reproductive function.
There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed.
Labor and Delivery:
Cefdinir has not been studied for use during labor and delivery.
Nursing Mothers:
Following administration of single 600 mg doses, cefdinir was not detected in human breast milk.
Pediatric Use:
Safety and efficacy in neonates and infants less than 6 months of age have not been established. Use of cefdinir for the treatment of acute maxillary sinusitis in pediatric patients (age 6 months through 12 years) is supported by evidence from adequate and well-controlled studies in adults and adolescents, the similar pathophysiology of acute sinusitis in adult and pediatric patients, and comparative pharmacokinetic data in the pediatric population.
Geriatric Use:
Efficacy is comparable in geriatric patients and younger adults. While cefdinir has been well-tolerated in all age groups, in clinical trials geriatric patients experienced a lower rate of adverse events, including diarrhea, than younger adults. Dose adjustment in elderly patients is not necessary unless renal function is markedly compromised (see DOSAGE AND ADMINISTRATION).
ADVERSE EVENTS
OVERDOSAGE
Information on cefdinir overdosage in humans is not available. In acute rodent toxicity studies, a single oral 5600 mg/kg dose produced no adverse effects. Toxic signs and symptoms following overdosage with other β- lactam antibiotics have included nausea, vomiting, epigastric distress, diarrhea, and convulsions. Hemodialysis removes cefdinir from the body. This may be useful in the event of a serious toxic reaction from overdosage, particularly if renal function is compromised.
CEFDINIR DOSAGE AND ADMINISTRATION
(see INDICATIONS AND USAGE for Indicated Pathogens)
The recommended dosage and duration of treatment for infections in adults and adolescents are described in the following chart; the total daily dose for all infections is 600 mg. Once-daily dosing for 10 days is as effective as BID dosing. Once-daily dosing has not been studied in pneumonia or skin infections; therefore, cefdinir capsules should be administered twice daily in these infections. Cefdinir capsules may be taken without regard to meals.
|
Type
of
Infection
|
Dosage
|
Duration
|
| Community-Acquired Pneumonia |
300 mg q12h |
10 days |
| Acute Exacerbations of Chronic Bronchitis |
300 mg q12h |
5 to 10 days |
|
|
or |
|
| Acute Maxillary Sinusitis |
600 mg q24h |
10 days |
|
|
300 mg q12h |
10 days |
|
|
or |
|
| Pharyngitis/Tonsillitis |
600 mg q24h |
10 days |
|
|
300 mg q12h |
5 to 10 days |
|
|
or |
|
| Uncomplicated Skin and Skin Structure Infections |
600 mg q24h |
10 days |
|
|
300 mg q12h |
10 days |
Patients With Renal Insufficiency:
For adult patients with creatinine clearance <30 mL/min, the dose of cefdinir should be 300 mg given once daily.
Creatinine clearance is difficult to measure in outpatients. However, the following formula may be used to estimate creatinine clearance (CLcr) in adult patients. For estimates to be valid, serum creatinine levels should reflect steady-state levels of renal function.
(weight) (140 – age)
Males: CLcr = ——————————
(72) (serum creatinine)
Females: CLcr = 0.85 x above value
where creatinine clearance is in mL/min, age is in years, weight is in kilograms, and serum creatinine is in mg/dL.(3)
The following formula may be used to estimate creatinine clearance in pediatric patients:
body length or height
CLcr = K x ——————————
serum creatinine
where K = 0.55 for pediatric patients older than 1 year(4) and 0.45 for infants (up to 1 year)(5).
In the above equation, creatinine clearance is in mL/min/1.73 m2, body length or height is in centimeters, and serum creatinine is in mg/dL.
For pediatric patients with a creatinine clearance of <30 mL/min/1.73 m2, the dose of cefdinir should be 7 mg/kg (up to 300 mg) given once daily.
Patients on Hemodialysis:
Hemodialysis removes cefdinir from the body. In patients maintained on chronic hemodialysis, the recommended initial dosage regimen is a 300 mg or 7 mg/kg dose every other day. At the conclusion of each hemodialysis session, 300 mg (or 7 mg/kg) should be given. Subsequent doses (300 mg or 7 mg/kg) are then administered every other day.
HOW SUPPLIED
Cefdinir capsules USP, 300 mg, size ‘0’ capsules having blue cap imprinted twice with "LUPIN" (in black ink) and purple body imprinted twice with "CEFDINIR" (in white ink) containing off white to creamish granular slug, are available as follows:
60 Capsules/Bottle NDC 68180-711-60
Store the capsules at 20°-25°C (68°-77°F); [see USP Controlled Room Temperature].
CLINICAL STUDIES
Community-Acquired Bacterial Pneumonia:
In a controlled, double-blind study in adults and adolescents conducted in the U.S., cefdinir BID was compared with cefaclor 500 mg TID. Using strict evaluability and microbiologic/clinical response criteria 6 to 14 days posttherapy, the following clinical cure rates, presumptive microbiologic eradication rates, and statistical outcomes were obtained:
|
|
Cefdinir
BID
|
Cefaclor
TID
|
Outcome
|
| Clinical Cure Rates Eradication Rates |
150/187 (80%) |
147/186 (79%) |
Cefdinir equivalent to control |
| Overall |
177/195 (91%) |
184/200 (92%) |
Cefdinir equivalent to control |
|
S
.
pneumoniae
|
31/31 (100%) |
35/35 (100%) |
|
|
H
.
influenzae
|
55/65 (85%) |
60/72 (83%) |
|
|
M
.
catarrhalis
|
10/10 (100%) |
11/11 (100%) |
|
|
H
.
parainfluenzae
|
81/89 (91%) |
78/82 (95%) |
|
In a second controlled, investigator-blind study in adults and adolescents conducted primarily in Europe, cefdinir BID was compared with amoxicillin/clavulanate 500/125 mg TID. Using strict evaluability and clinical response criteria 6 to 14 days posttherapy, the following clinical cure rates, presumptive microbiologic eradication rates, and statistical outcomes were obtained:
|
|
Cefdinir
BID
|
Amoxicillin
/
Clavulanate TID |
Outcome
|
| Clinical Cure Rates Eradication Rates |
83/104 (80%) |
86/97 (89%) |
Cefdinir not equivalent to control |
| Overall |
85/96 (89%) |
84/90 (93%) |
Cefdinir equivalent to control |
|
S
.
pneumoniae
|
42/44 (95%) |
43/44 (98%) |
|
|
H
.
influenzae
|
26/35 (74%) |
21/26 (81%) |
|
|
M
.
catarrhalis
|
6/6 (100%) |
8/8 (100%) |
|
|
H
.
parainfluenzae
|
11/11 (100%) |
12/12 (100%) |
|
Streptococcal Pharyngitis/Tonsillitis:
In four controlled studies conducted in the U.S., cefdinir was compared with 10 days of penicillin in adult, adolescent, and pediatric patients. Two studies (one in adults and adolescents, the other in pediatric patients) compared 10 days of cefdinir QD or BID to penicillin 250 mg or 10 mg/kg QID. Using strict evaluability and microbiologic/clinical response criteria 5 to 10 days posttherapy, the following clinical cure rates, microbiologic eradication rates, and statistical outcomes were obtained:
|
Study
|
Efficacy
Parameter
|
Cefdinir
QD
|
Cefdinir
BID
|
Penicillin
QID
|
Outcome
|
| Adults/ Adolescents |
Eradication of S
.
pyogenes
|
192/210 (91%) |
199/217 (92%) |
181/217 (83%) |
Cefdinir superior to control |
|
|
Clinical Cure Rates |
199/210 (95%) |
209/217 (96%) |
193/217 (89%) |
Cefdinir superior to control |
| Pediatric Patients |
Eradication of S
.
pyogenes
|
215/228 (94%) |
214/227 (94%) |
159/227 (70%) |
Cefdinir superior to control |
|
|
Clinical Cure Rates |
222/228 (97%) |
218/227 (96%) |
196/227 (86%) |
Cefdinir superior to control |
Two studies (one in adults and adolescents, the other in pediatric patients) compared 5 days of cefdinir BID to 10 days of penicillin 250 mg or 10 mg/kg QID. Using strict evaluability and microbiologic/ clinical response criteria 4 to 10 days posttherapy, the following clinical cure rates, microbiologic eradication rates, and statistical outcomes were obtained:
|
Study
|
Efficacy
Parameter
|
Cefdinir
BID
|
Penicillin
QID
|
Outcome
|
| Adults/ Adolescents |
Eradication of S
.
pyogenes
|
193/218 (89%) |
176/214 (82%) |
Cefdinir equivalent to control |
|
|
Clinical Cure Rates |
194/218 (89%) |
181/214 (85%) |
Cefdinir equivalent to control |
| Pediatric Patients |
Eradication of S
.
pyogenes
|
176/196 (90%) |
135/193 (70%) |
Cefdinir superior to control |
|
|
Clinical Cure Rates |
179/196 (91%) |
173/193 (90%) |
Cefdinir equivalent to control |
REFERENCES
- National Committee for Clinical Laboratory Standards. Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically, 4th ed. Approved Standard, NCCLS Document M7-A4, Vol 17(2). NCCLS, Villanova, PA, Jan 1997.
- National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Disk Susceptibility Tests, 6th ed. Approved Standard, NCCLS Document M2-A6, Vol 17(1). NCCLS, Villanova, PA, Jan 1997.
- Cockcroft DW, Gault MH. Prediction of creatinine clearance from serum creatinine. Nephron, 1976;16:31-41.
- Schwartz GJ, Haycock GB, Edelmann CM, Spitzer A. A simple estimate of glomerular filtration rate in children derived from body length and plasma creatinine. Pediatrics 1976;58:259-63.
- Schwartz GJ, Feld LG, Langford DJ. A simple estimate of glomerular filtration rate in full-term infants during the first year of life. J Pediatrics 1984;104:849-54.
Manufactured for:
Lupin Pharmaceuticals, Inc.
Baltimore, Maryland 21202
United States
Manufactured by:
Lupin Limited
Mandideep 462 046
INDIA
Maalox® is a registered trademark of Rhone-Poulenc Rorer.
Clinistix® and Clinitest® are registered trademarks of Miles Diagnostics.
Tes-tape® is a registered trademark of Lilly.
Revised 15th December 2009 ID#:218628
PRINCIPAL DISPLAY PANEL
NDC 54569-5921-1
Relabeled by:
A-S Medication Solutions
Libertyville, IL 60048

CefdinirCefdinir CAPSULE
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||