ESZOPICLONE
Bryant Ranch Prepack
Bryant Ranch Prepack
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use eszopiclone safely and effectively. See full prescribing information for eszopiclone tablets.Eszopiclone Tablets for oral use CIVInitial U.S. Approval: 2004 INDICATIONS AND USAGEEszopiclone tablets are indicated for the treatment of insomnia. Eszopiclone tablets have been shown to decrease sleep latency and improve sleep maintenance.DOSAGE AND ADMINISTRATION Non Elderly Adult dose: starting dose 2 mg immediately before bedtime. Can be started at or raised to 3 mg if clinically indicated since 3 mg is more effective for sleep maintenance (2.1) Elderly: for difficulty falling asleep 1 mg immediately before bedtime. For difficulty staying asleep 2mg immediately before bedtime (2.1) Severe Hepatic Impairment: Starting dose 1 mg. Use with caution in these patients (2.1) Starting dose should not exceed 1 mg in patients coadministered eszopiclone tablets with potent CYP3A4 inhibitors. Maximum dose is 2 mg (2.1) Should not be taken with or immediately after a meal (2.1) DOSAGE FORMS AND STRENGTHS1 mg, 2 mg, and 3 mg tablets (3).CONTRAINDICATIONSKnown hypersensitivity to eszopiclone (4)WARNINGS AND PRECAUTIONS Evaluate for co-morbid diagnoses: Reevaluate if insomnia persists after 7 to 10 days of use (5.1) Severe anaphalactic/anaphylactoid reactions: Angioedema and anaphylaxis have been reported. Do not rechallenge if such reactions occur (5.2) Abnormal thinking, behavioral changes and complex behaviors: May include “sleep-driving” and hallucinations. Immediately evaluate any new onset behavioral changes (5.3) Depression: Worsening of depression or suicidal thinking may occur. Prescribe the least number of tablets feasible to avoid intentional overdose (5.3, 5.7) Withdrawal effects: symptoms may occur with rapid dose reduction or discontinuation (5.4, 9.3) CNS depressant effects: Use can impair alertness and motor coordination. If used in combination with other CNS depressants, dose reductions may be needed due to additive effects. Do not take together with ethanol (5.5, 5.7) Elderly/debilitated patients: Use lower dose due to impaired motor, cognitive performance and increased sensitivity (2.1, 5.7) Patients with hepatic impairment, compromised respiratory function, impaired drug metabolism or hemodynamic responses: Use with caution (5.7) Side EffectsMost commonly observed adverse reactions (incidence ≥2%) were unpleasant taste, headache, somnolence, respiratory infection, dizziness, dry mouth, rash, anxiety, hallucinations, and viral infections To report SUSPECTED ADVERSE REACTIONS, contact CARACO Pharmaceutical Laboratories Ltd. at 1-800-818-4555 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. DRUG INTERACTIONS CNS depressants: Additive CNS-depressant effects with combination use. Use with ethanol causes additive psychomotor impairment (7.1) Rifampicin: Combination use may decrease exposure to and effects of eszopiclone (7.2) Ketoconazole: Combination use increases exposure to and effect of eszopiclone. Dose reduction of eszopiclone is needed (7.2) USE IN SPECIFIC POPULATIONS Pregnancy: Based on animal data, may cause fetal harm (8.1) Pediatric use: Safety and effectiveness not established. The labeling for Sunovion Pharmaceutical Inc.’s eszopiclone tablets includes additional information from a clinical study in which efficacy was not demonstrated in pediatric patients. However, due to Sunovion Pharmaceuticals, Inc.’s marketing exclusivity rights, this drug product is not labeled with that pediatric information. (8.4).
FULL PRESCRIBING INFORMATION: CONTENTS*
- 1 ESZOPICLONE INDICATIONS AND USAGE
- 2 ESZOPICLONE DOSAGE AND ADMINISTRATION
- 3 DOSAGE FORMS AND STRENGTHS
- 4 ESZOPICLONE CONTRAINDICATIONS
- 5 WARNINGS AND PRECAUTIONS
- 6 ESZOPICLONE ADVERSE REACTIONS
- 7 DRUG INTERACTIONS
- 8 USE IN SPECIFIC POPULATIONS
- 9 DRUG ABUSE AND DEPENDENCE
- 10 OVERDOSAGE
- 11 ESZOPICLONE DESCRIPTION
- 12 CLINICAL PHARMACOLOGY
- 13 NONCLINICAL TOXICOLOGY
- 14 CLINICAL STUDIES
- 16 HOW SUPPLIED/STORAGE AND HANDLING
- 17 PATIENT COUNSELING INFORMATION
- Medication Guide
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
Eszopiclone tablets are indicated for the treatment of insomnia. In controlled outpatient and sleep laboratory studies, eszopiclone tablets administered at bedtime decreased sleep latency and improved sleep maintenance.
The clinical trials performed in support of efficacy were up to 6 months in duration. The final formal assessments of sleep latency and maintenance were performed at 4 weeks in the 6-week study (adults only), at the end of both 2-week studies (elderly only) and at the end of the 6-month study (adults only).
2 DOSAGE AND ADMINISTRATION
2.1 Dosage in Adults
The dose of eszopiclone tablets should be individualized. The recommended starting dose for eszopiclone tablets for most non-elderly adults is 2 mg immediately before bedtime. Dosing can be initiated at or raised to 3 mg if clinically indicated, since 3 mg is more effective for sleep maintenance [see Warnings and Precautions (5)].
Use in Geriatric Patients
The recommended starting dose of eszopiclone tablets for elderly patients whose primary complaint is difficulty falling asleep is 1 mg immediately before bedtime. In these patients, the dose may be increased to 2 mg if clinically indicated. For elderly patients whose primary complaint is difficulty staying asleep, the recommended dose is 2 mg immediately before bedtime [see Warnings and Precautions: Special Populations (5.7)].
Use in Patients with Hepatic Impairment
The starting dose of eszopiclone tablets should be 1 mg in patients with severe hepatic impairment. Eszopiclone tablets should be used with caution in these patients.
Use with CYP3A4 Inhibitors
The starting dose of eszopiclone tablets should not exceed 1 mg in patients coadministered eszopiclone tablets with potent CYP3A4 inhibitors. If needed, the dose can be raised to 2 mg.
Use with CNS depressants
Dosage adjustments may be necessary when eszopiclone tablets are combined with other CNS depressant drugs because of the potentially additive effects [see Warnings and Precautions (5.5)].
Administration with Food
Taking eszopiclone tablets with or immediately after a heavy, high-fat meal results in slower absorption and would be expected to reduce the effect of eszopiclone tablets on sleep latency [see Clinical Pharmacology: Pharmacokinetics (12.3)].
3 DOSAGE FORMS AND STRENGTHS
Eszopiclone tablets are available in 1 mg, 2 mg and 3 mg strengths for oral administration.
Eszopiclone tablets 1 mg are blue colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘1’ on other side.
Eszopiclone tablets 2 mg are white colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘2’ on other side.
Eszopiclone tablets 3 mg are dark blue colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘3’ on other side.
4 CONTRAINDICATIONS
Eszopiclone is contraindicated in patients with known hypersensitivity to eszopiclone. Hypersensitivity reactions include anaphylaxis and angioedema [see Warnings and Precautions (5.2)].
5 WARNINGS AND PRECAUTIONS
5.1 Need to evaluate for co-morbid diagnoses
Because sleep disturbances may be the presenting manifestation of a physical and/or psychiatric disorder, symptomatic treatment of insomnia should be initiated only after a careful evaluation of the patient. The failure of insomnia to remit after 7 to 10 days of treatment may indicate the presence of a primary psychiatric and/or medical illness that should be evaluated . Worsening of insomnia or the emergence of new thinking or behavior abnormalities may be the consequence of an unrecognized psychiatric or physical disorder. Such findings have emerged during the course of treatment with sedative/hypnotic drugs, including eszopiclone. Because some of the important adverse effects of eszopiclone appear to be dose-related, it is important to use the lowest possible effective dose, especially in the elderly [see Dosage and Administration (2)].
5.2 Severe anaphylactic and anaphylactoid reactions
Rare cases of angioedema involving the tongue, glottis or larynx have been reported in patients after taking the first or subsequent doses of sedative-hypnotics, including eszopiclone. Some patients have had additional symptoms such as dyspnea, throat closing, or nausea and vomiting that suggest anaphylaxis. Some patients have required medical therapy in the emergency department. If angioedema involves the tongue, glottis or larynx, airway obstruction may occur and be fatal. Patients who develop angioedema after treatment with eszopiclone should not be rechallenged with the drug.
5.3 Abnormal Thinking and Behavioral Changes
A variety of abnormal thinking and behavior changes have been reported to occur in association with the use of sedative/hypnotics. Some of these changes may be characterized by decreased inhibition (e.g., aggressiveness and extroversion that seem out of character), similar to effects produced by alcohol and other CNS depressants. Other reported behavioral changes have included bizarre behavior, agitation, hallucinations, and depersonalization. Amnesia and other neuropsychiatric symptoms may occur unpredictably. In primarily depressed patients, worsening of depression, including suicidal thoughts and actions (including completed suicides), has been reported in association with the use of sedative/hypnotics.
Complex behaviors such as “sleep-driving” (i.e., driving while not fully awake after ingestion of a sedative-hypnotic, with amnesia for the event) have been reported. These events can occur in sedative-hypnotic-naïve as well as in sedative-hypnotic-experienced persons. Although behaviors such as sleep-driving may occur with eszopiclone alone at therapeutic doses, the use of alcohol and other CNS depressants with eszopiclone appears to increase the risk of such behaviors, as does the use of eszopiclone at doses exceeding the maximum recommended dose. Due to the risk to the patient and the community, discontinuation of eszopiclone should be strongly considered for patients who report a “sleep-driving” episode. Other complex behaviors (e.g., preparing and eating food, making phone calls, or having sex) have been reported in patients who are not fully awake after taking a sedative-hypnotic. As with sleep-driving, patients usually do not remember these events.
It can rarely be determined with certainty whether a particular instance of the abnormal behaviors listed above are drug-induced, spontaneous in origin, or a result of an underlying psychiatric or physical disorder. Nonetheless, the emergence of any new behavioral sign or symptom of concern requires careful and immediate evaluation.
5.4 Withdrawal Effects
Following rapid dose decrease or abrupt discontinuation of the use of sedative/hypnotics, there have been reports of signs and symptoms similar to those associated with withdrawal from other CNS-depressant drugs [see Drug Abuse and Dependence (9)].
5.5 CNS Depressant Effects
Eszopiclone, like other hypnotics, has CNS-depressant effects. Because of the rapid onset of action, eszopiclone should only be ingested immediately prior to going to bed or after the patient has gone to bed and has experienced difficulty falling asleep. Patients receiving eszopiclone should be cautioned against engaging in hazardous occupations requiring complete mental alertness or motor coordination (e.g., operating machinery or driving a motor vehicle) after ingesting the drug, and be cautioned about potential impairment of the performance of such activities on the day following ingestion of eszopiclone. Eszopiclone, like other hypnotics, may produce additive CNS-depressant effects when coadministered with other psychotropic medications, anticonvulsants, antihistamines, ethanol, and other drugs that themselves produce CNS depression. Eszopiclone should not be taken together with alcohol. Dose adjustment may be necessary when eszopiclone is administered with other CNS-depressant agents, because of the potentially additive effects.
5.6 Timing of Drug Administration
Eszopiclone should be taken immediately before bedtime. Taking a sedative/hypnotic while still up and about may result in short-term memory impairment, hallucinations, impaired coordination, dizziness, and lightheadedness.
5.7 Special Populations
Use in Elderly and/or Debilitated Patients
Impaired motor and/or cognitive performance after repeated exposure or unusual sensitivity to sedative/hypnotic drugs is a concern in the treatment of elderly and/or debilitated patients. The recommended starting dose of eszopiclone for these patients is 1 mg [see Dosage and Administration (2)]
.
Use in Patients with Concomitant Illness
Clinical experience with eszopiclone in patients with concomitant illness is limited. Eszopiclone should be used with caution in patients with diseases or conditions that could affect metabolism or hemodynamic responses.
A study in healthy volunteers did not reveal respiratory-depressant effects at doses 2.5-fold higher (7 mg) than the recommended dose of eszopiclone. Caution is advised, however, if eszopiclone is prescribed to patients with compromised respiratory function.
The dose of eszopiclone should be reduced to 1 mg in patients with severe hepatic impairment, because systemic exposure is doubled in such subjects. No dose adjustment appears necessary for subjects with mild or moderate hepatic impairment. No dose adjustment appears necessary in subjects with any degree of renal impairment, since less than 10% of eszopiclone is excreted unchanged in the urine.
The dose of eszopiclone should be reduced in patients who are administered potent inhibitors of CYP3A4, such as ketoconazole, while taking eszopiclone. Downward dose adjustment is also recommended when eszopiclone is administered with agents having known CNS-depressant effects.
Use in Patients with Depression
Sedative/hypnotic drugs should be administered with caution to patients exhibiting signs and symptoms of depression. Suicidal tendencies may be present in such patients, and protective measures may be required. Intentional overdose is more common in this group of patients; therefore, the least amount of drug that is feasible should be prescribed for the patient at any one time.
6 ADVERSE REACTIONS
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice. The premarketing development program for eszopiclone included eszopiclone exposures in patients and/or normal subjects from two different groups of studies: approximately 400 normal subjects in clinical pharmacology/pharmacokinetic studies, and approximately 1550 patients in placebo-controlled clinical effectiveness studies, corresponding to approximately 263 patient-exposure years. The conditions and duration of treatment with eszopiclone varied greatly and included (in overlapping categories) open-label and double-blind phases of studies, inpatients and outpatients, and short-term and longer-term exposure. Adverse reactions were assessed by collecting adverse events, results of physical examinations, vital signs, weights, laboratory analyses, and ECGs.
Adverse reactions during exposure were obtained primarily by general inquiry and recorded by clinical investigators using terminology of their own choosing. Consequently, it is not possible to provide a meaningful estimate of the proportion of individuals experiencing adverse reactions without first grouping similar types of events into a smaller number of standardized event categories. In the tables and tabulations that follow, COSTART terminology has been used to classify reported adverse reactions.
The stated frequencies of adverse reactions represent the proportion of individuals who experienced, at least once, adverse reaction of the type listed. A reaction was considered treatment-emergent if it occurred for the first time or worsened while the patient was receiving therapy following baseline evaluation.
6.1 Adverse Findings Observed in Placebo-Controlled Trials
Adverse Reactions Resulting in Discontinuation of Treatment
In placebo-controlled, parallel-group clinical trials in the elderly, 3.8% of 208 patients who received placebo, 2.3% of 215 patients who received 2 mg eszopiclone, and 1.4% of 72 patients who received 1 mg eszopiclone discontinued treatment due to an adverse reaction. In the 6-week parallel-group study in adults, no patients in the 3 mg arm discontinued because of an adverse reaction. In the long-term 6-month study in adult insomnia patients, 7.2% of 195 patients who received placebo and 12.8% of 593 patients who received 3 mg eszopiclone discontinued due to an adverse reaction. No reaction that resulted in discontinuation occurred at a rate of greater than 2%.
Adverse Reactions Observed at an Incidence of ≥2% in Controlled Trials
Table 1 shows the incidence of adverse reactions from a Phase 3 placebo-controlled study of eszopiclone at doses of 2 or 3 mg in non-elderly adults. Treatment duration in this trial was 44 days. The table includes only reactions that occurred in 2% or more of patients treated with eszopiclone 2 mg or 3 mg in which the incidence in patients treated with eszopiclone was greater than the incidence in placebo-treated patients.
|
Adverse Reaction
|
Placebo
(n=99) |
Eszopiclone
2 mg (n=104) |
Eszopiclone
3 mg (n=105) |
| Body as a Whole |
|||
| Headache |
13 |
21 |
17 |
| Viral Infection |
1 |
3 |
3 |
| Digestive System |
|||
| Dry Mouth |
3 |
5 |
7 |
| Dyspepsia |
4 |
4 |
5 |
| Nausea |
4 |
5 |
4 |
| Vomiting |
1 |
3 |
0 |
| Nervous System |
|||
| Anxiety |
0 |
3 |
1 |
| Confusion |
0 |
0 |
3 |
| Depression |
0 |
4 |
1 |
| Dizziness |
4 |
5 |
7 |
| Hallucinations |
0 |
1 |
3 |
| Libido Decreased |
0 |
0 |
3 |
| Nervousness |
3 |
5 |
0 |
| Somnolence |
3 |
10 |
8 |
| Respiratory System |
|||
| Infection |
3 |
5 |
10 |
| Skin and Appendages |
|||
| Rash |
1 |
3 |
4 |
| Special Senses |
|||
| Unpleasant Taste |
3 |
17 |
34 |
| Urogenital System |
|||
Dysmenorrhea |
0 |
3 |
0 |
Gynecomastia |
0 |
3 |
0 |
Adverse reactions from Table 1 that suggest a dose-response relationship in adults include viral infection, dry mouth, dizziness, hallucinations, infection, rash, and unpleasant taste, with this relationship clearest for unpleasant taste.
Table 2 shows the incidence of adverse reactions from combined Phase 3 placebo-controlled studies of eszopiclone at doses of 1 or 2 mg in elderly adults (ages 65 to 86). Treatment duration in these trials was 14 days. The table includes only reactions that occurred in 2% or more of patients treated with eszopiclone 1 mg or 2 mg in which the incidence in patients treated with eszopiclone was greater than the incidence in placebo-treated patients.
|
Adverse Reactions
|
Placebo
(n=208) |
Eszopiclone
1 mg (n=72) |
Eszopiclone
2 mg (n=215) |
| Body as a Whole |
|||
| Accidental Injury |
1 |
0 |
3 |
| Headache |
14 |
15 |
13 |
| Pain |
2 |
4 |
5 |
| Digestive System |
|||
| Diarrhea |
2 |
4 |
2 |
| Dry Mouth |
2 |
3 |
7 |
| Dyspepsia |
2 |
6 |
2 |
| Nervous System |
|||
| Abnormal Dreams |
0 |
3 |
1 |
| Dizziness |
2 |
1 |
6 |
| Nervousness |
1 |
0 |
2 |
| Neuralgia |
0 |
3 |
0 |
| Skin and Appendages |
|||
| Pruritus |
1 |
4 |
1 |
| Special Senses |
|||
| Unpleasant Taste |
0 |
8 |
12 |
| Urogenital System |
|||
| Urinary Tract Infection |
0 |
3 |
0 |
Adverse reactions from Table 2 that suggest a dose-response relationship in elderly adults include pain, dry mouth, and unpleasant taste, with this relationship again clearest for unpleasant taste.
These figures cannot be used to predict the incidence of adverse reactions in the course of usual medical practice because patient characteristics and other factors may differ from those that prevailed in the clinical trials. Similarly, the cited frequencies cannot be compared with figures obtained from other clinical investigations involving different treatments, uses, and investigators. The cited figures, however, do provide the prescribing physician with some basis for estimating the relative contributions of drug and non-drug factors to the adverse reaction incidence rate in the population studied.
Other Reactions Observed During the Premarketing Evaluation of Eszopiclone
Following is a list of modified COSTART terms that reflect adverse reactions as defined in the introduction to the Adverse Reactions section and reported by approximately 1550 subjects treated with eszopiclone at doses in the range of 1 to 3.5 mg/day during Phase 2 and 3 clinical trials throughout the United States and Canada. All reported reactions are included except those already listed in Tables 1 and 2 or elsewhere in labeling, minor reactions common in the general population, and reactions unlikely to be drug-related. Although the reactions reported occurred during treatment with eszopiclone, they were not necessarily caused by it.
Reactions are further categorized by body system and listed in order of decreasing frequency according to the following definitions: frequent adverse reactions are those that occurred on one or more occasions in at least 1/100 patients; infrequent adverse reactions are those that occurred in fewer than 1/100 patients but in at least 1/1,000 patients; rare adverse reactions are those that occurred in fewer than 1/1,000 patients. Gender-specific reactions are categorized based on their incidence for the appropriate gender.
Body as a Whole: Frequent: chest pain; Infrequent:allergic reaction, cellulitis, face edema, fever, halitosis, heat stroke, hernia, malaise, neck rigidity, photosensitivity.
Cardiovascular System: Frequent: migraine; Infrequent: hypertension; Rare:thrombophlebitis.
Digestive System: Infrequent: anorexia,
cholelithiasis, increased appetite, melena, mouth ulceration, thirst, ulcerative stomatitis; Rare: colitis, dysphagia, gastritis, hepatitis, hepatomegaly, liver damage, stomach ulcer, stomatitis, tongue edema, rectal hemorrhage.
Hemic and Lymphatic System: Infrequent: anemia, lymphadenopathy.
Metabolic and Nutritional: Frequent: peripheral edema; Infrequent: hypercholesteremia, weight gain, weight loss; Rare: dehydration, gout, hyperlipemia, hypokalemia.
Musculoskeletal System: Infrequent: arthritis, bursitis, joint disorder (mainly swelling, stiffness, and pain), leg cramps, myasthenia, twitching; Rare: arthrosis, myopathy, ptosis.
Nervous System: Infrequent: agitation, apathy, ataxia, emotional lability, hostility, hypertonia, hypesthesia, incoordination, insomnia, memory impairment, neurosis, nystagmus, paresthesia, reflexes decreased, thinking abnormal (mainly difficulty concentrating), vertigo; Rare: abnormal gait, euphoria, hyperesthesia, hypokinesia, neuritis, neuropathy, stupor, tremor.
Respiratory System: Infrequent: asthma, bronchitis, dyspnea, epistaxis, hiccup, laryngitis.
Skin and Appendages: Infrequent: acne, alopecia, contact dermatitis, dry skin, eczema, skin discoloration, sweating, urticaria; Rare: erythema multiforme, furunculosis, herpes zoster, hirsutism, maculopapular rash, vesiculobullous rash.
Special Senses: Infrequent: conjunctivitis, dry eyes, ear pain, otitis externa, otitis media, tinnitus, vestibular disorder; Rare: hyperacusis, iritis, mydriasis, photophobia.
Urogenital System: Infrequent: amenorrhea,
breast engorgement, breast enlargement, breast neoplasm, breast pain, cystitis, dysuria, female lactation, hematuria, kidney calculus, kidney pain, mastitis, menorrhagia, metrorrhagia, urinary frequency, urinary incontinence, uterine hemorrhage, vaginal hemorrhage, vaginitis; Rare: oliguria, pyelonephritis, urethritis.
7 DRUG INTERACTIONS
7.1 CNS Active Drugs
Ethanol: An additive effect on psychomotor performance was seen with coadministration of eszopiclone and ethanol
Olanzapine: Coadministration of eszopiclone and olanzapine produced a decrease in DSST scores. The interaction was pharmacodynamic; there was no alteration in the pharmacokinetics of either drug.
7.2 Drugs that Inhibit or Induce CYP3A4
Drugs That Inhibit CYP3A4 (Ketoconazole)
CYP3A4 is a major metabolic pathway for elimination of eszopiclone. The exposure of eszopiclone was increased by coadministration of ketoconazole, a potent inhibitor of CYP3A4. Other strong inhibitors of CYP3A4 (e.g., itraconazole, clarithromycin, nefazodone, troleandomycin, ritonavir, nelfinavir) would be expected to behave similarly. Dose reduction of eszopiclone is needed for patient coadministered with potent CYP3A4 inhibitors. [see Dosage and Administration (2.1)]
Drugs that Induce CYP3A4 (Rifampicin)
Racemic zopiclone exposure was decreased 80% by concomitant use of rifampicin, a potent inducer of CYP3A4. A similar effect would be expected with eszopiclone. Combination use with CYP3A4 inducer may decrease exposure to and effects of eszopiclone.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category C
There are no adequate and well-controlled studies in pregnant women. Eszopiclone should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Oral administration of eszopiclone to pregnant rats (62.5, 125, or 250 mg/kg/day) and rabbits (4, 8, or 16 mg/kg/day) throughout organogenesis showed no evidence of teratogenicity up to the highest doses tested. In rats, reduced fetal weight and increased incidences of skeletal variations and/or delayed ossification were observed at the mid and high doses. The no-observed-effect dose for adverse effects on embryofetal development is 200 times the maximum recommended human dose (MRHD) of 3 mg/day on a mg/m2 basis. No effects on embryofetal development were observed in rabbits; the highest dose tested is approximately 100 times the MRHD on a mg/m2 basis.
Oral administration of eszopiclone (60, 120, or 180 mg/kg/day) to pregnant rats throughout the pregnancy and lactation resulted in increased post-implantation loss, decreased postnatal pup weights and survival, and increased pup startle response at all doses. The lowest dose tested is approximately 200 times the MRHD on a mg/m2 basis. Eszopiclone had no effects on other developmental measures or reproductive function in the offspring.
8.3 Nursing Mothers
It is not known whether this drug is excreted in human milk.
8.4 Pediatric Use
Safety and effectiveness have not been established in pediatric patients.
The labeling for Sunovion Pharmaceutical Inc.’s eszopiclone tablets includes additional information from a clinical study in which efficacy was not demonstrated in pediatric patients. However, due to Sunovion Pharmaceuticals, Inc.’s marketing exclusivity rights, this drug product is not labeled with that pediatric information.
In studies in which eszopiclone (2 to 300 mg/kg/day) was orally administered to young rats from weaning through sexual maturity, neurobehavioral impairment (altered auditory startle response) and reproductive toxicity (adverse effects on male reproductive organ weights and histopathology) were observed at doses ≥ 5 mg/kg/day. Delayed sexual maturation was noted in males and females at ≥ 10 mg/kg/day. The no-effect dose (2 mg/kg) was associated with plasma exposures (AUC) for eszopiclone and metabolite (S)-desmethylzopiclone [(S)-DMZ] approximately 2 times plasma exposures in humans at the maximum recommended dose (MRHD) in adults (3 mg/day).
When eszopiclone (doses from 1 to 50 mg/kg/day) was orally administered to young dogs from weaning through sexual maturity, neurotoxicity (convulsions) was observed at doses ≥ 5 mg/kg/day. Hepatotoxicity (elevated liver enzymes and hepatocellular vacuolation and degeneration) and reproductive toxicity (adverse effects on male reproductive organ weights and histopathology) were noted at dose ≥ 10 mg/kg/day. The no-effect dose (1 mg/kg) was associated with plasma exposures (AUC) to eszopiclone and (S)-DMZ approximately 3 and 2 times, respectively, plasma exposures in humans at the MRHD in adults.
8.5 Geriatric Use
A total of 287 subjects in double-blind, parallel-group, placebo-controlled clinical trials who received eszopiclone were 65 to 86 years of age. The overall pattern of adverse events for elderly subjects (median age = 71 years) in 2-week studies with nighttime dosing of 2 mg eszopiclone was not different from that seen in younger adults [see Adverse Reactions: Table 2 (6)]. Eszopiclone 2 mg exhibited significant reduction in sleep latency and improvement in sleep maintenance in the elderly population. Compared with non-elderly adults, subjects 65 years and older had longer elimination and higher total exposure to eszopiclone. Therefore, dose reduction is recommended in the elderly patients [see Dosage and Administration (2.1), Clinical Pharmacology (12.3)].
8.6 Hepatic Impairment
No dose adjustment is necessary for patients with mild-to-moderate hepatic impairment. Exposure was increased in severely impaired patients compared with the healthy volunteers. The starting dose of eszopiclone should be 1 mg in patients with severe hepatic impairment. Eszopiclone should be used with caution in patients with hepatic impairment [see Dosage and Administration (2.1), Clinical Pharmacology (12.3)].
9 DRUG ABUSE AND DEPENDENCE
9.1 Controlled Substance
Eszopiclone is a Schedule IV controlled substance under the Controlled Substances Act. Other substances under the same classification are benzodiazepines and the nonbenzodiazepine hypnotics zaleplon and zolpidem. While eszopiclone is a hypnotic agent with a chemical structure unrelated to benzodiazepines, it shares some of the pharmacologic properties of the benzodiazepines.
9.2 Abuse
Abuse and addiction are separate and distinct from physical dependence and tolerance. Abuse is characterized by misuse of the drug for non-medical purposes, often in combination with other psychoactive substances. Physical dependence is a state of adaptation that is manifested by a specific withdrawal syndrome that can be produced by abrupt cessation, rapid dose reduction, decreasing blood level of the drug and/or administration of an antagonist. Tolerance is a state of adaptation in which exposure to a drug induces changes that result in a diminution of one or more of the drug’s effects over time. Tolerance may occur to both the desired and undesired effects of drugs and may develop at different rates for different effects.
Addiction is a primary, chronic, neurobiological disease with genetic, psychosocial, and environmental factors influencing its development and manifestations. It is characterized by behaviors that include one or more of the following: impaired control over drug use, compulsive use, continued use despite harm, and craving. Drug addiction is a treatable disease, utilizing a multidisciplinary approach, but relapse is common.
In a study of abuse liability conducted in individuals with known histories of benzodiazepine abuse, eszopiclone at doses of 6 and 12 mg produced euphoric effects similar to those of diazepam 20 mg. In this study, at doses 2-fold or greater than the maximum recommended doses, a dose-related increase in reports of amnesia and hallucinations was observed for both eszopiclone and diazepam.
9.3 Dependence
The clinical trial experience with eszopiclone revealed no evidence of a serious withdrawal syndrome. Nevertheless, the following adverse events included in DSM-IV criteria for uncomplicated sedative/hypnotic withdrawal were reported during clinical trials following placebo substitution occurring within 48 hours following the last eszopiclone treatment: anxiety, abnormal dreams, nausea, and upset stomach. These reported adverse events occurred at an incidence of 2% or less. Use of benzodiazepines and similar agents may lead to physical and psychological dependence. The risk of abuse and dependence increases with the dose and duration of treatment and concomitant use of other psychoactive drugs. The risk is also greater for patients who have a history of alcohol or drug abuse or history of psychiatric disorders. These patients should be under careful surveillance when receiving eszopiclone or any other hypnotic.
9.4 Tolerance
Some loss of efficacy to the hypnotic effect of benzodiazepines and benzodiazepine-like agents may develop after repeated use of these drugs for a few weeks.
No development of tolerance to any parameter of sleep measurement was observed over six months. Tolerance to the efficacy of eszopiclone 3 mg was assessed by 4-week objective and 6‑week subjective measurements of time to sleep onset and sleep maintenance for eszopiclone in a placebo-controlled 44-day study, and by subjective assessments of time to sleep onset and WASO in a placebo-controlled study for 6 months.
10 OVERDOSAGE
In clinical trials with eszopiclone, one case of overdose with up to 36 mg of eszopiclone was reported in which the subject fully recovered. Since commercial marketing began, spontaneous cases of eszopiclone overdoses up to 270 mg (90 times the maximum recommended dose of eszopiclone) have been reported, in which patients have recovered. Fatalities related to eszopiclone overdoses were reported only in combination with other CNS drugs or alcohol.
10.1 Signs and Symptoms
Signs and symptoms of overdose effects of CNS depressants can be expected to present as exaggerations of the pharmacological effects noted in preclinical testing. Impairment of consciousness ranging from somnolence to coma has been described. Rare individual instances of fatal outcomes following overdose with racemic zopiclone have been reported in European postmarketing reports, most often associated with overdose with other CNS-depressant agents.
10.2 Recommended Treatment
General symptomatic and supportive measures should be used along with immediate gastric lavage where appropriate. Intravenous fluids should be administered as needed. Flumazenil may be useful. As in all cases of drug overdose, respiration, pulse, blood pressure, and other appropriate signs should be monitored and general supportive measures employed. Hypotension and CNS depression should be monitored and treated by appropriate medical intervention. The value of dialysis in the treatment of overdosage has not been determined.
As with the management of all overdosage, the possibility of multiple drug ingestion should be considered. The physician may wish to consider contacting a poison control center for up-to-date information on the management of hypnotic drug product overdosage.
11 DESCRIPTION
Eszopiclone is a nonbenzodiazepine hypnotic agent that is a pyrrolopyrazine derivative of the cyclopyrrolone class. The chemical name of eszopiclone is (+)-(5S)-6-(5-chloropyridin-2-yl)-7-oxo-6,7-dihydro-5H-pyrrolo[3,4-b] pyrazin-5-yl 4-methylpiperazine-1-carboxylate. Its molecular weight is 388.82, and its empirical formula is C17H17ClN6O3. Eszopiclone has a single chiral center with an (S)-configuration. It has the following chemical structure:
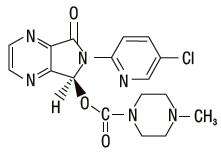
Eszopiclone is a white to light-yellow crystalline solid. Eszopiclone is very slightly soluble in water, slightly soluble in ethanol, and soluble in phosphate buffer (pH 3.2).
Eszopiclone is formulated as film-coated tablets for oral administration. Eszopiclone tablets contain 1 mg, 2 mg, or 3 mg eszopiclone and the following inactive ingredients: microcrystalline cellulose, pregelatinized starch, anhydrous lactose, croscarmellose sodium, colloidal silicon dioxide, magnesium stearate, titanium dioxide, hypromellose, polyethylene glycol, polysorbate 80 (for 1 mg & 2 mg), FD&C Blue #2 (for 1 mg & 3 mg), FD&C Yellow #6 (for 3 mg) and FD&C Red #40 (for 3 mg).
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
The precise mechanism of action of eszopiclone as a hypnotic is unknown, but its effect is believed to result from its interaction with GABA-receptor complexes at binding domains located close to or allosterically coupled to benzodiazepine receptors. Eszopiclone is a nonbenzodiazepine hypnotic that is a pyrrolopyrazine derivative of the cyclopyrrolone class with a chemical structure unrelated to pyrazolopyrimidines, imidazopyridines, benzodiazepines, barbiturates, or other drugs with known hypnotic properties.
12.3 Pharmacokinetics
The pharmacokinetics of eszopiclone have been investigated in healthy subjects (adult and elderly) and in patients with hepatic disease or renal disease. In healthy subjects, the pharmacokinetic profile was examined after single doses of up to 7.5 mg and after once-daily administration of 1, 3, and 6 mg for 7 days. Eszopiclone is rapidly absorbed, with a time to peak concentration (tmax) of approximately 1 hour and a terminal-phase elimination half-life (t1/2) of approximately 6 hours. In healthy adults, eszopiclone does not accumulate with once-daily administration, and its exposure is dose-proportional over the range of 1 to 6 mg.
Absorption and Distribution
Eszopiclone
is rapidly absorbed following oral administration. Peak plasma concentrations are achieved within approximately 1 hour after oral administration. Eszopiclone is weakly bound to plasma protein (52 to 59%). The large free fraction suggests that eszopiclone disposition should not be affected by drug-drug interactions caused by protein binding. The blood-to-plasma ratio for eszopiclone is less than one, indicating no selective uptake by red blood cells.
Metabolism
Following oral administration, eszopiclone is extensively metabolized by oxidation and demethylation. The primary plasma metabolites are (S)-zopiclone-N-oxide and (S)-N-desmethyl zopiclone; the latter compound binds to GABA receptors with substantially lower potency than eszopiclone, and the former compound shows no significant binding to this receptor. In vitro studies have shown that CYP3A4 and CYP2E1 enzymes are involved in the metabolism of eszopiclone. Eszopiclone did not show any inhibitory potential on CYP450 1A2, 2A6, 2C9, 2C19, 2D6, 2E1, and 3A4 in cryopreserved human hepatocytes.
Elimination
After oral administration, eszopiclone is eliminated with a mean t1/2of approximately 6 hours. Up to 75% of an oral dose of racemic zopiclone is excreted in the urine, primarily as metabolites. A similar excretion profile would be expected for eszopiclone, the S-isomer of racemic zopiclone. Less than 10% of the orally administered eszopiclone dose is excreted in the urine as parent drug.
Effect of Food
In healthy adults, administration of a 3 mg dose of eszopiclone after a high-fat meal resulted in no change in AUC, a reduction in mean Cmax of 21%, and delayed tmax by approximately 1 hour. The half-life remained unchanged, approximately 6 hours. The effects of eszopiclone on sleep onset may be reduced if it is taken with or immediately after a high-fat/heavy meal.
Specific Populations
Age
Compared with non-elderly adults, subjects 65 years and older had an increase of 41% in total exposure (AUC) and a slightly prolonged elimination of eszopiclone (t1/2 approximately 9 hours). Cmax was unchanged. Therefore, in elderly patients the starting dose of eszopiclone should be decreased to 1 mg and the dose should not exceed 2 mg.
Gender
The pharmacokinetics of eszopiclone in men and women are similar.
Race
In an analysis of data on all subjects participating in Phase 1 studies of eszopiclone, the pharmacokinetics for all races studied appeared similar.
Hepatic impairment
Pharmacokinetics of a 2 mg eszopiclone dose were assessed in 16 healthy volunteers and in 8 subjects with mild, moderate, and severe liver disease. Exposure was increased 2-fold in severely impaired patients compared with the healthy volunteers. Cmax and tmax were unchanged. No dose adjustment is necessary for patients with mild-to-moderate hepatic impairment. Dose reduction is recommended for patients with severe hepatic impairment. Eszopiclone should be used with caution in patients with hepatic impairment [see Dosage and Administration (2.1)].
Renal Impairment
The pharmacokinetics of eszopiclone were studied in 24 patients with mild, moderate, or severe renal impairment. AUC and Cmax were similar in the patients compared with demographically matched healthy control subjects. No dose adjustment is necessary in patients with renal impairment, since less than 10% of the orally administered eszopiclone dose is excreted in the urine as parent drug.
Drug Interactions
Eszopiclone is metabolized by CYP3A4 and CYP2E1 via demethylation and oxidation. There were no pharmacokinetic or pharmacodynamic interactions between eszopiclone and paroxetine. When eszopiclone was coadministered with olanzapine, no pharmacokinetic interaction was detected in levels of eszopiclone or olanzapine, but a pharmacodynamic interaction was seen on a measure of psychomotor function. Eszopiclone and lorazepam decreased each other’s Cmax by 22%. Coadministration of eszopiclone 3 mg to subjects receiving ketoconazole, a potent inhibitor of CYP3A4, 400 mg daily for 5 days, resulted in a 2.2-fold increase in exposure to eszopiclone. Cmax and t1/2 were increased 1.4-fold and 1.3-fold, respectively. Eszopiclone would not be expected to alter the clearance of drugs metabolized by common CYP450 enzymes [see Warnings and Precautions: Special Populations (5.7),
Dosage and Administration (2.1)
].
Paroxetine: Coadministration of single dose of eszopiclone and paroxetine produced no pharmacokinetic or pharmacodynamic interaction. The lack of a drug interaction following single-dose administration does not predict the complete absence of a pharmacodynamic effect following chronic administration.
Lorazepam: Coadministration of single doses of eszopiclone and lorazepam did not have clinically relevant effects on the pharmacodynamics or pharmacokinetics of either drug. The lack of a drug interaction following single-dose administration does not predict the complete absence of a pharmacodynamic effect following chronic administration.
Drugs with a Narrow Therapeutic Index
Digoxin: A single dose of eszopiclone 3 mg did not affect the pharmacokinetics of digoxin measured at steady state following dosing of 0.5 mg twice daily for one day and 0.25 mg daily for the next 6 days.
Warfarin: Eszopiclone 3 mg administered daily for 5 days did not affect the pharmacokinetics of (R)- or (S)-warfarin, nor were there any changes in the pharmacodynamic profile (prothrombin time) following a single 25 mg oral dose of warfarin.
Drugs Highly Bound to Plasma Protein
Eszopiclone is not highly bound to plasma proteins (52 to 59% bound); therefore, the disposition of eszopiclone is not expected to be sensitive to alterations in protein binding. Administration of eszopiclone 3 mg to a patient taking another drug that is highly protein-bound would not be expected to cause an alteration in the free concentration of either drug.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, mutagenesis, impairment of fertility
Carcinogenesis
In a carcinogenicity study in rats, oral administration of eszopiclone for 97 (males) or 104 (females) weeks resulted in no increases in tumors; plasma levels (AUC) of eszopiclone at the highest dose tested (16 mg/kg/day) are approximately 80 (females) and 20 (males) times those in humans at the maximum recommended human dose (MRHD) of 3 mg/day. However, in a 2-year carcinogenicity study in rats, oral administration of racemic zopiclone (1, 10, or 100 mg/kg/day) resulted in increases in mammary gland adenocarcinomas (females) and thyroid gland follicular cell adenomas and carcinomas (males) at the highest dose tested. Plasma levels of eszopiclone at this dose are approximately 150 (females) and 70 (males) times those in humans at the MRHD of eszopiclone. The mechanism for the increase in mammary adenocarcinomas is unknown. The increase in thyroid tumors is thought to be due to increased levels of TSH secondary to increased metabolism of circulating thyroid hormones, a mechanism not considered relevant to humans.
In a 2-year carcinogenicity study in mice, oral administration of racemic zopiclone (1, 10, or 100 mg/kg/day) produced increases in pulmonary carcinomas and carcinomas plus adenomas (females) and skin fibromas and sarcomas (males) at the highest dose tested. The skin tumors were due to skin lesions induced by aggressive behavior, a mechanism not relevant to humans. A carcinogenicity study of eszopiclone was conducted in mice at oral doses up to 100 mg/kg/day. Although this study did not reach a maximum tolerated dose, and was thus inadequate for overall assessment of carcinogenic potential, no increases in either pulmonary or skin tumors were seen at doses producing plasma levels of eszopiclone approximately 90 times those in humans at the MRHD of eszopiclone (and 12 times the exposure in the racemate study).
Eszopiclone did not increase tumors in a p53 transgenic mouse bioassay at oral doses up to 300 mg/kg/day.
Mutagenesis
Eszopiclone was clastogenic in in vitro (mouse lymphoma and chromosomal aberration) assays in mammalian cells. Eszopiclone was negative in the in vitro bacterial gene mutation (Ames) assay and in an in vivo micronucleus assay.
(S)-N-desmethyl zopiclone, a metabolite of eszopiclone, was positive in in vitro chromosomal aberration assays in mammalian cells. (S)-N-desmethyl zopiclone was negative in the in vitro bacterial gene mutation (Ames) assay and in an in vivo chromosomal aberration and micronucleus assay.
Impairment of Fertility
Oral administration of eszopiclone to rats prior to and during mating, and continuing in females to day 7 of gestation (doses up to 45 mg/kg/day to males and females or up to 180 mg/kg/day to females only) resulted in decreased fertility, with no pregnancy at the highest dose tested when both males and females were treated. In females, there was an increase in abnormal estrus cycles at the highest dose tested. In males, decreases in sperm number and motility and increases in morphologically abnormal sperm were observed at the mid and high doses. The no-effect dose for adverse effects on fertility (5 mg/kg/day) is 16 times the MRHD on a mg/m2 basis.
14 CLINICAL STUDIES
The effect of eszopiclone on reducing sleep latency and improving sleep maintenance was established in studies with 2100 subjects (ages 18 to 86) with chronic and transient insomnia in six placebo-controlled trials of up to 6 months’ duration. Two of these trials were in elderly patients (n=523). Overall, at the recommended adult dose (2 to 3 mg) and elderly dose (1 to 2 mg), eszopiclone significantly decreased sleep latency and improved measures of sleep maintenance (objectively measured as wake time after sleep onset [WASO] and subjectively measured as total sleep time).
14.1 Transient Insomnia
Healthy adults were evaluated in a model of transient insomnia (n=436) in a sleep laboratory in a double-blind, parallel-group, single-night trial comparing two doses of eszopiclone and placebo. Eszopiclone 3 mg was superior to placebo on measures of sleep latency and sleep maintenance, including polysomnographic (PSG) parameters of latency to persistent sleep (LPS) and WASO.
14.2 Chronic Insomnia (Adults and Elderly)
The effectiveness of eszopiclone was established in five controlled studies in chronic insomnia. Three controlled studies were in adult subjects, and two controlled studies were in elderly subjects with chronic insomnia.
Adults
In the first study, adults with chronic insomnia (n=308) were evaluated in a double-blind, parallel-group trial of 6 weeks’ duration comparing eszopiclone 2 mg and 3 mg with placebo. Objective endpoints were measured for 4 weeks. Both 2 mg and 3 mg were superior to placebo on LPS at 4 weeks. The 3 mg dose was superior to placebo on WASO.
In the second study, adults with chronic insomnia (n=788) were evaluated using subjective measures in a double-blind, parallel-group trial comparing the safety and efficacy of eszopiclone 3 mg with placebo administered nightly for 6 months. Eszopiclone was superior to placebo on subjective measures of sleep latency, total sleep time, and WASO.
In addition, a 6-period cross-over PSG study evaluating eszopiclone doses of 1 to 3 mg, each given over a 2-day period, demonstrated effectiveness of all doses on LPS, and of 3 mg on WASO. In this trial, the response was dose-related.
Elderly
Elderly subjects (ages 65 to 86) with chronic insomnia were evaluated in two double-blind, parallel-group trials of 2 weeks duration. One study (n=231) compared the effects of eszopiclone with placebo on subjective outcome measures, and the other (n=292) on objective and subjective outcome measures. The first study compared 1 mg and 2 mg of eszopiclone with placebo, while the second study compared 2 mg of eszopiclone with placebo. All doses were superior to placebo on measures of sleep latency. In both studies, 2 mg of eszopiclone was superior to placebo on measures of sleep maintenance.
14.3 Studies Pertinent to Safety Concerns for Sedative Hypnotic Drugs
Cognitive, Memory, Sedative, and Psychomotor Effects
In two double-blind, placebo-controlled, single-dose cross-over studies of 12 patients each (one study in patients with insomnia; one in normal volunteers), the effects of eszopiclone 2 and 3 mg were assessed on 20 measures of cognitive function and memory at 9.5 and 12 hours after a nighttime dose. Although results suggested that patients receiving eszopiclone 3 mg performed more poorly than patients receiving placebo on a very small number of these measures at 9.5 hours post-dose, no consistent pattern of abnormalities was seen.
In a 6-month double-blind, placebo-controlled trial of nightly administered eszopiclone 3 mg, 8/593 subjects treated with eszopiclone 3 mg (1.3%) and 0/195 subjects treated with placebo (0%) spontaneously reported memory impairment. The majority of these events were mild in nature (5/8), and none were reported as severe. Four of these events occurred within the first 7 days of treatment and did not recur. The incidence of spontaneously reported confusion in this 6-month study was 0.5% in both treatment arms. In a 6-week adult study of nightly administered eszopiclone 2 mg or 3 mg or placebo, the spontaneous reporting rates for confusion were 0%, 3%, and 0%, respectively, and for memory impairment were 1%, 1%, and 0%, respectively.
In a 2-week study of 264 elderly insomniacs randomized to either nightly eszopiclone 2 mg or placebo, spontaneous reporting rates of confusion and memory impairment were 0% vs. 0.8% and 1.5% vs. 0%, respectively. In another 2-week study of 231 elderly insomniacs, the spontaneous reporting rates for the 1 mg, 2 mg, and placebo groups for confusion were 0%, 2.5%, and 0%, respectively, and for memory impairment were 1.4%, 0%, and 0%, respectively.
A study of normal subjects exposed to single fixed doses of eszopiclone from 1 to 7.5 mg using the DSST to assess sedation and psychomotor function at fixed times after dosing (hourly up to 16 hours) found the expected sedation and reduction in psychomotor function. This was maximal at 1 hour and present up to 4 hours, but was no longer present by 5 hours.
In another study, patients with insomnia were given 2 or 3 mg doses of eszopiclone nightly, with DSST assessed on the mornings following days 1, 15, and 29 of treatment. While both the placebo and eszopiclone 3 mg groups showed an improvement in DSST scores relative to baseline the following morning (presumably due to a learning effect), the improvement in the placebo group was greater and reached statistical significance on night 1, although not on nights 15 and 29. For the eszopiclone 2 mg group, DSST change scores were not significantly different from placebo at any time point.
Withdrawal-Emergent Anxiety and Insomnia
During nightly use for an extended period, pharmacodynamic tolerance or adaptation has been observed with other hypnotics. If a drug has a short elimination half-life, it is possible that a relative deficiency of the drug or its active metabolites (i.e., in relationship to the receptor site) may occur at some point in the interval between each night’s use. This is believed to be responsible for two clinical findings reported to occur after several weeks of nightly use of other rapidly eliminated hypnotics: increased wakefulness during the last quarter of the night and the appearance of increased signs of daytime anxiety.
In a 6-month double-blind, placebo-controlled study of nightly administration of eszopiclone 3 mg, rates of anxiety reported as an adverse event were 2.1% in the placebo arm and 3.7% in the eszopiclone arm. In a 6-week adult study of nightly administration, anxiety was reported as an adverse event in 0%, 2.9%, and 1% of the placebo, 2 mg, and 3 mg treatment arms, respectively. In this study, single-blind placebo was administered on nights 45 and 46, the first and second days of withdrawal from study drug. New adverse events were recorded during the withdrawal period, beginning with day 45, up to 14 days after discontinuation. During this withdrawal period, 105 subjects previously taking nightly eszopiclone 3 mg for 44 nights spontaneously reported anxiety (1%), abnormal dreams (1.9%), hyperesthesia (1%), and neurosis (1%), while none of 99 subjects previously taking placebo reported any of these adverse events during the withdrawal period.
Rebound insomnia, defined as a dose-dependent temporary worsening in sleep parameters (latency, sleep efficiency, and number of awakenings) compared with baseline following discontinuation of treatment, is observed with short- and intermediate-acting hypnotics. Rebound insomnia following discontinuation of eszopiclone relative to placebo and baseline was examined objectively in a 6-week adult study on the first 2 nights of discontinuation (nights 45 and 46) following 44 nights of active treatment with 2 mg or 3 mg. In the eszopiclone 2 mg group, compared with baseline, there was a significant increase in WASO and a decrease in sleep efficiency, both occurring only on the first night after discontinuation of treatment. No changes from baseline were noted in the eszopiclone 3 mg group on the first night after discontinuation, and there was a significant improvement in LPS and sleep efficiency compared with baseline following the second night of discontinuation. Comparisons of changes from baseline between eszopiclone and placebo were also performed. On the first night after discontinuation of eszopiclone 2 mg, LPS and WASO were significantly increased and sleep efficiency was reduced; there were no significant differences on the second night. On the first night following discontinuation of eszopiclone 3 mg, sleep efficiency was significantly reduced. No other differences from placebo were noted in any other sleep parameter on either the first or second night following discontinuation. For both doses, the discontinuation-emergent effect was mild, had the characteristics of the return of the symptoms of chronic insomnia, and appeared to resolve by the second night after eszopiclone discontinuation.
16 HOW SUPPLIED/STORAGE AND HANDLING
Eszopiclone tablets 1 mg are blue colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘1’ on other side.
Bottles of 30’s with Child Resistant Cap……………..NDC 47335-586-83
Bottles of 100’s with Child Resistant Cap……………NDC 47335-586-88
Bottles of 100’s with Non Child Resistant Cap………NDC 47335-586-08
Bottles of 1000’s with Non Child Resistant Cap……..NDC 47335-586-18
Eszopiclone tablets 2 mg are white colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘2’ on other side.
Bottles of 30’s with Child Resistant Cap……………..NDC 47335-587-83
Bottles of 100’s with Child Resistant Cap……………NDC 47335-587-88
Bottles of 100’s with Non Child Resistant Cap………NDC 47335-587-08
Bottles of 1000’s with Non Child Resistant Cap……..NDC 47335-587-18
Eszopiclone tablets 3 mg are dark blue colored, circular, film-coated tablets, debossed with ‘S’ on one side and ‘3’ on other side.
Bottles of 30’s with Child Resistant Cap……………..NDC 47335-588-83
Bottles of 100’s with Child Resistant Cap……………NDC 47335-588-88
Bottles of 100’s with Non Child Resistant Cap………NDC 47335-588-08
Bottles of 1000’s with Non Child Resistant Cap……..NDC 47335-588-18
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Dispense in tight container with child-resistant closure.
17 PATIENT COUNSELING INFORMATION
Patients should be instructed to read the accompanying Medication Guide with each new prescription and refill. The complete text of the Medication Guide is reprinted at the end of this document. Patients should be given the following information:
Severe anaphylactic and anaphylactoid reactions
Inform patients that severe anaphylactic and anaphylactoid reactions have occurred with eszopiclone tablets. Describe the signs/symptoms of these reactions and advise patients to seek medical attention immediately if any of them occur.
“Sleep-Driving” and other complex behaviors
There have been reports of people getting out of bed after taking a sedative-hypnotic and driving their cars while not fully awake, often with no memory of the event. If a patient experiences such an episode, it should be reported to his or her doctor immediately, since “sleep-driving” can be dangerous. This behavior is more likely to occur when eszopiclone tablets are taken with alcohol or other central nervous system depressants [see Warnings and Precautions (5.3)]. Other complex behaviors (e.g., preparing and eating food, making phone calls, or having sex) have been reported in patients who are not fully awake after taking a sedative-hypnotic. As with sleep-driving, patients usually do not remember these events.
Administration instructions
- Patients should be instructed to take eszopiclone tablets immediately prior to going to bed, and only if they can dedicate 8 hours to sleep.
- Patients should be instructed not to take eszopiclone tablets with alcohol or with other sedating medications.
- Patients should be advised to consult with their physician if they have a history of depression, mental illness, or suicidal thoughts, have a history of drug or alcohol abuse, or have liver disease.
- Women should be advised to contact their physician if they become pregnant, plan to become pregnant, or if they are nursing.
Medication Guide
Eszopiclone Tablets C-IV
Read the Medication Guide that comes with eszopiclone tablets before you start taking it and each time you get a refill. There may be new information. This Medication Guide does not take the place of talking to your doctor about your medical condition or treatment.
What is the most important information I should know about eszopiclone tablets?
After taking eszopiclone tablets, you may get up out of bed while not being fully awake and do an activity that you do not know you are doing. The next morning, you may not remember that you did anything during the night. You have a higher chance for doing these activities if you drink alcohol or take other medicines that make you sleepy with eszopiclone tablets. Reported activities include:
- driving a car ("sleep-driving")
- making and eating food
- talking on the phone
- having sex
- sleep-walking
Call your doctor right away if you find out that you have done any of the above activities after taking eszopiclone tablets.
Important:
1. Take eszopiclone tablets exactly as prescribed
- Do not take more eszopiclone tablets than prescribed.
- Take eszopiclone tablets right before you get in bed, not sooner.
2. Do not take eszopiclone tablets if you:
- drink alcohol
- take other medicines that can make you sleepy. Talk to your doctor about all of your medicines. Your doctor will tell you if you can take eszopiclone tablets with your other medicines
- cannot get a full night’s sleep
WHAT ARE ESZOPICLONE TABLETS?
Eszopiclone tablets are sedative-hypnotic (sleep) medicines. Eszopiclone tablets are used in adults for the treatment of a sleep problem called insomnia. Symptoms of insomnia include:
- trouble falling asleep
- waking up often during the night
Eszopiclone tablets arenot for children.
|
Eszopiclone is a federally controlled substance (C-IV) because it can be abused or lead to dependence. Keep eszopiclone tablets in a safe place to prevent misuse and abuse. Selling or giving away eszopiclone tablets may harm others, and is against the law. Tell your doctor if you have ever abused or been dependent on alcohol, prescription medicines or street drugs. |
Who should not take eszopiclone tablets?
Do not take eszopiclone tablets if you are allergic to anything in it.
See the end of this Medication Guide for a complete list of ingredients in eszopiclone tablets.
Eszopiclone tablets may not be right for you. Before starting eszopiclone tablets, tell your doctor about all of your health conditions, including if you:
- have a history of depression, mental illness, or suicidal thoughts
- have a history of drug or alcohol abuse or addiction
- have liver disease
- are pregnant, planning to become pregnant, or breastfeeding
Tell your doctor about all of the medicines you take including prescription and nonprescription medicines, vitamins and herbal supplements. Medicines can interact with each other, sometimes causing serious side effects. Do not take eszopiclone tablets with other medicines that can make you sleepy.
Know the medicines you take. Keep a list of your medicines with you to show your doctor and pharmacist each time you get a new medicine.
How should I take eszopiclone tablets?
- Take eszopiclone tablets exactly as prescribed. Do not take more eszopiclone tablets than prescribed for you.
- Take eszopiclone tablets right before you get into bed.
- Do not take eszopiclone tablets with or right after a meal.
- Do not take eszopiclone tablets unless you are able to get a full night’s sleep before you must be active again.
- Call your doctor if your insomnia worsens or is not better within 7 to 10 days. This may mean that there is another condition causing your sleep problems.
- If you take too many eszopiclone tablets or overdose, call your doctor or poison control center right away, or get emergency treatment.
What are the possible side effects of eszopiclone tablets?
Possible serious side effects of eszopiclone tablets include:
- getting out of bed while not being fully awake and do an activity that you do not know you are doing. (See “What is the most important information I should know about eszopiclone tablets?)
- abnormal thoughts and behavior. Symptoms include more outgoing or aggressive behavior than normal, confusion, agitation, hallucinations, worsening of depression, and suicidal thoughts or actions.
- memory loss
- anxiety
- severe allergic reactions. Symptoms include swelling of the tongue or throat, trouble breathing, and nausea and vomiting. Get emergency medical help if you get these symptoms after taking eszopiclone tablets .
Call your doctor right away if you have any of the above side effects or any other side effects that worry you while using eszopiclone tablets.
The most common side effects of eszopiclone tablets are:
- unpleasant taste in mouth, dry mouth
- drowsiness
- dizziness
- headache
- symptoms of the common cold
- You may still feel drowsy the next day after taking eszopiclone tablets . Do not drive or do other dangerous activities after taking eszopiclone tablets until you feel fully awake.
These are not all the side effects ofeszopiclone tablets. Ask your doctor or pharmacist for more information. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I Store Eszopiclone Tablets?
- Store eszopiclone tablets at room temperature 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F).
- Do not use eszopiclone tablets after the expiration date.
- Keep eszopiclone tablets and all medicines out of reach of children.
General Information about Eszopiclone Tablets
- Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide.
- Do not use eszopiclone tablets for a condition for which it was not prescribed.
- Do not share eszopiclone tablets with other people, even if you think they have the same symptoms that you have. It may harm them and is against the law.
This Medication Guide summarizes the most important information abouteszopiclone tablets. If you would like more information, talk with your doctor. You can ask your doctor or pharmacist for information abouteszopiclone tabletsthat is written for healthcare professionals.
For customer service, reporting side effects and medical information; call 1-800-818-4555.
What are the ingredients in eszopiclone tablets?
Active Ingredient: eszopiclone.
Inactive Ingredients: microcrystalline cellulose, pregelatinized starch, anhydrous lactose, croscarmellose sodium, colloidal silicon dioxide, magnesium stearate, titanium dioxide, hypromellose, polyethylene glycol, polysorbate 80 (for 1 mg & 2 mg), FD&C Blue #2 (for 1 mg & 3 mg), FD&C Yellow #6 (for 3 mg) and FD&C Red #40 (for 3 mg).
This Medication Guide has been approved by the U.S. Food and Drug Administration.
Distributed by:
Caraco Pharmaceutical Laboratories, Ltd.
1150 Elijah McCoy Drive, Detroit, MI 48202
Manufactured by:
Sun Pharma Laboratories Limited
Survey No. 259/15,
Dadra-396 191 (U.T. of D & NH), India.
PGPI0252
ISS. 01/2014
Eszopiclone 2mg (CIV) Tablet
ESZOPICLONEESZOPICLONE TABLET, FILM COATED
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||