levofloxacin
Torrent Pharmaceuticals Limited
Torrent Pharma, Inc.
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use levofloxacin tablets safely and effectively. See full prescribing information for levofloxacin tablets. Levofloxacin TabletsRx OnlyInitial U.S. Approval: 1996BOXED WARNING WARNING: Fluoroquinolones, including levofloxacin, are associated with an increased risk of tendinitis and tendon rupture in all ages. This risk is further increased in older patients usually over 60 years of age, in patients taking corticosteroid drugs, and in patients with kidney, heart or lung transplants [See Warnings and Precautions (5.1)]. Fluoroquinolones, including levofloxacin, may exacerbate muscle weakness in persons with myasthenia gravis. Avoid levofloxacin in patients with a known history of myasthenia gravis [See Warnings and Precautions (5.2)]. To reduce the development of drug-resistant bacteria and maintain the effectiveness of levofloxacin and other antibacterial drugs, levofloxacin tablets should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria.RECENT MAJOR CHANGESWarnings and Precautions Exacerbation of myasthenia gravis (5.2) 01/2011 INDICATIONS AND USAGELevofloxacin tablets are a fluoroquinolone antibacterial indicated in adults (≥18 years of age) with infections caused by designated, susceptible bacteria (1, 12.4). Pneumonia: nosocomial (1.1) and community acquired (1.2, 1.3) Acute bacterial sinusitis (1.4) Acute bacterial exacerbation of chronic bronchitis (1.5) Skin and skin structure infections: complicated (1.6) and uncomplicated (1.7) Chronic bacterial prostatitis (1.8) Urinary tract infections: complicated (1.9, 1.10) and uncomplicated (1.12) Acute pyelonephritis (1.11) Inhalational anthrax, post-exposure (1.13). Not tested in humans for post- exposure prevention of inhalational anthrax; plasma concentrations are likely to predict efficacy (14.9) DOSAGE AND ADMINISTRATION Dosage in patients with normal renal function (2.1) Type of Infection Dose Every 24 hours Duration ( days ) Nosocomial Pneumonia (1.1) 750 mg 7-14 Community Acquired Pneumonia (1.2) 500 mg 7-14 Community Acquired Pneumonia (1.3) 750 mg 5 Acute Bacterial Sinusitis (1.4) 750 mg 5 500 mg 10-14 Acute Bacterial Exacerbation of Chronic Bronchitis (1.5)24 500 mg 7 Complicated Skin and Skin Structure Infections (SSSI) (1.6) 750 mg 7-14 Uncomplicated SSSI (1.7) 500 mg 7-10 Chronic Bacterial Prostatitis (1.8) 500 mg 28 Complicated Urinary Tract Infection (1.9) or Acute Pyelonephritis (1.11) 750 mg 5 Complicated Urinary Tract Infection (1.10) or Acute Pyelonephritis (1.11) 250 mg 10 Uncomplicated Urinary Tract Infection (1.12) 250 mg 3 Inhalational Anthrax (Post-Exposure) (1.13) Adult and pediatric patients > 50 kg and ≥ 6 months of age Pediatric patients < 50 kg and ≥ 6 months of age 500 mg 8 mg/kg BID(not to exceed250mg/dose) 60 60 Adjust dose for creatinine clearance < 50 mL/min (2.3, 8.6, 12.3) DOSAGE FORMS AND STRENGTHS Formulation ( 3 ) Strength Tablets 250 mg, 500 mg, and 750 mg CONTRAINDICATIONSKnown hypersensitivity to levofloxacin or other quinolones (4, 5.3)WARNINGS AND PRECAUTIONS Risk of tendinitis and tendon rupture is increased. This risk is further increased in older patients usually over 60 years of age, in patients taking corticosteroids, and in patients with kidney, heart or lung transplants. Discontinue if pain or inflammation in a tendon occurs (5.1, 8.5) May exacerbate muscle weakness in persons with myasthenia gravis. Avoid use in patients with a known history of myasthenia gravis (5.2). Anaphylactic reactions and allergic skin reactions, serious, occasionally fatal, may occur after first dose (4, 5.3) Hematologic (including agranulocytosis, thrombocytopenia), and renal toxicities may occur after multiple doses (5.4) Hepatotoxicity: Severe, and sometimes fatal, hepatoxicity has been reported. Discontinue immediately if signs and symptoms of hepatitis occur (5.5) Central nervous system effects, including convulsions, anxiety, confusion, depression, and insomnia may occur after the first dose. Use with caution in patients with known or suspected disorders that may predispose them to seizures or lower the seizure threshold (5.6) Clostridium difficile-associated colitis: evaluate if diarrhea occurs (5.7) Peripheral neuropathy: discontinue if symptoms occur in order to prevent irreversibility (5.8) Prolongation of the QT interval and isolated cases of torsade de pointes have been reported. Avoid use in patients with known prolongation, those with hypokalemia, and with other drugs that prolong the QT interval (5.9, 8.5) Side EffectsThe most common reactions (≥ 3%) were nausea, headache, diarrhea, insomnia, constipation and dizziness (6.2). To report SUSPECTED ADVERSE REACTIONS, contact Torrent Pharma Inc. at 1-269-544-2299 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. DRUG INTERACTIONS Interacting Drug Interaction Multivalent cation-containing products including antacids, metal cation or didanosine Absorption of levofloxacin is decreased when the tablet formulation is taken within 2 hours of these products. Warfarin Effect may be enhanced. Monitor prothrombin time, INR, watch for bleeding (7.2) Antidiabetic agent Carefully monitor blood glucose (5.11, 7.3) USE IN SPECIFIC POPULATIONS Geriatrics: Severe hepatotoxicity has been reported. The majority of reports describe patients 65 years of age or older (5.5, 8.5, 17). May have increased risk of tendinopathy (including rupture), especially with concomitant corticosteroid use (5.1, 8.5, 17). May be more susceptible to prolongation of the QT interval. (5.9, 8.5, 17). Pediatrics: Musculoskeletal disorders (arthralgia, arthritis, tendinopathy, and gait abnormality) seen in more levofloxacin-treated patients than in comparator. Shown to cause arthropathy and osteochondrosis in juvenile animals (5.10, 8.4, 13.2). Safety in pediatrics patients treated for more than 14 days has not been studied. Risk-benefit appropriate only for the treatment of inhalation anthrax (post-exposure) (1.13, 2.2, 8.4, 14.9)
FULL PRESCRIBING INFORMATION: CONTENTS*
- 1. LEVOFLOXACIN INDICATIONS AND USAGE
- 1.1 Nosocomial Pneumonia
- 1.2 Community-Acquired Pneumonia: 7-14 day Treatment Regimen
- 1.3 Community-Acquired Pneumonia: 5-day Treatment Regimen
- 1.4 Acute Bacterial Sinusitis: 5-day and 10-14 day Treatment Regimens
- 1.5 Acute Bacterial Exacerbation of Chronic Bronchitis
- 1.6 Complicated Skin and Skin Structure Infections
- 1.7 Uncomplicated Skin and Skin Structure Infections
- 1.8 Chronic Bacterial Prostatitis
- 1.9 Complicated Urinary Tract Infections: 5-day Treatment Regimen
- 1.10 Complicated Urinary Tract Infections: 10-day Treatment Regimen
- 1.11 Acute Pyelonephritis: 5 or 10-day Treatment Regimen
- 1.12 Uncomplicated Urinary Tract Infections
- 1.13 Inhalational Anthrax (Post-Exposure)
- 2. LEVOFLOXACIN DOSAGE AND ADMINISTRATION
- 3. DOSAGE FORMS AND STRENGTHS
- 4. LEVOFLOXACIN CONTRAINDICATIONS
- 5. WARNINGS AND PRECAUTIONS
- 5.1 Tendinopathy and Tendon Rupture
- 5.2 Exacerbation of Myasthenia Gravis
- 5.3 Hypersensitivity Reactions
- 5.4 Other Serious and Sometimes Fatal Reactions
- 5.5 Hepatotoxicity
- 5.6 Central Nervous System Effects
- 5.7 Clostridium difficile-Associated Diarrhea
- 5.8 Peripheral Neuropathy
- 5.9 Prolongation of the QT Interval
- 5.10 Musculoskeletal Disorders in Pediatric Patients and Arthropathic Effects in Animals
- 5.11 Blood Glucose Disturbances
- 5.12 Photosensitivity/Phototoxicity
- 5.13 Development of Drug Resistant Bacteria
- 6. LEVOFLOXACIN ADVERSE REACTIONS
- 7. DRUG INTERACTIONS
- 8. USE IN SPECIFIC POPULATIONS
- 10. OVERDOSAGE
- 11. LEVOFLOXACIN DESCRIPTION
- 12. CLINICAL PHARMACOLOGY
- 13. NONCLINICAL TOXICOLOGY
- 14. CLINICAL STUDIES
- 14.1 Nosocomial Pneumonia
- 14.2 Community-Acquired Pneumonia: 7-14 day Treatment Regimen
- 14.3 Community-Acquired Pneumonia: 5-Day Treatment Regimen
- 14.4 Acute Bacterial Sinusitis: 5-day and 10-14 day Treatment Regimens
- 14.5 Complicated Skin and Skin Structure Infections
- 14.6 Chronic Bacterial Prostatitis
- 14.7 Complicated Urinary Tract Infections and Acute Pyelonephritis: 5-day Treatment Regimen
- 14.8 Complicated Urinary Tract Infections and Acute Pyelonephritis: 10-day Treatment Regimen
- 14.9 Inhalational Anthrax (Post-Exposure)
- 15. REFERENCES
- 16. HOW SUPPLIED/STORAGE AND HANDLING
- 17. PATIENT COUNSELING INFORMATION
- PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
FULL PRESCRIBING INFORMATION
WARNING:
Fluoroquinolones, including levofloxacin, are associated with an increased risk of tendinitis and tendon rupture in all ages. This risk is further increased in older patients usually over 60 years of age, in patients taking corticosteroid drugs, and in patients with kidney, heart or lung transplants [See Warnings and Precautions (5.1)].
Fluoroquinolones, including levofloxacin, may exacerbate muscle weakness in persons with myasthenia gravis. Avoid levofloxacin in patients with a known history of myasthenia gravis [See Warnings and Precautions (5.2)].
1. INDICATIONS AND USAGE
To reduce the development of drug-resistant bacteria and maintain the effectiveness of levofloxacin tablets and other antibacterial drugs, levofloxacin tablets should be used only to treat or prevent infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Levofloxacin tablets are indicated for the treatment of adults (≥ 18 years of age) with mild, moderate, and severe infections caused by susceptible strains of the designated microorganisms in the conditions listed in this section.
Culture and susceptibility testing
Appropriate culture and susceptibility tests should be performed before treatment in order to isolate and identify organisms causing the infection and to determine their susceptibility to levofloxacin [see Clinical Pharmacology (12.4)]. Therapy with levofloxacin tablets may be initiated before results of these tests are known; once results become available, appropriate therapy should be selected.
As with other drugs in this class, some strains of Pseudomonas aeruginosa may develop resistance fairly rapidly during treatment with levofloxacin tablets. Culture and susceptibility testing performed periodically during therapy will provide information about the continued susceptibility of the pathogens to the antimicrobial agent and also the possible emergence of bacterial resistance.
1.1 Nosocomial Pneumonia
Levofloxacin tablets are indicated for the treatment of nosocomial pneumonia due to methicillin-susceptible Staphylococcus aureus, Pseudomonas aeruginosa, Serratia marcescens, Escherichia coli, Klebsiella pneumoniae, Haemophilus influenzae, or Streptococcus pneumoniae. Adjunctive therapy should be used as clinically indicated. Where Pseudomonas aeruginosa is a documented or presumptive pathogen, combination therapy with an anti-pseudomonal β-lactam is recommended [see Clinical Studies (14.1)].
1.2 Community-Acquired Pneumonia: 7-14 day Treatment Regimen
Levofloxacin tablets are indicated for the treatment of community-acquired pneumonia due to methicillin-susceptible Staphylococcus aureus, Streptococcus pneumoniae (including multi-drug-resistant Streptococcus pneumoniae [MDRSP]), Haemophilus influenzae, Haemophilus parainfluenzae, Klebsiella pneumoniae, Moraxella catarrhalis, Chlamydophila pneumoniae, Legionella pneumophila, or Mycoplasma pneumoniae [see Dosage and Administration (2.1) and Clinical Studies (14.2)].
MDRSP isolates are strains resistant to two or more of the following antibacterials: penicillin (MIC ≥ 2 mcg/mL), 2nd generation cephalosporins, e.g., cefuroxime, macrolides, tetracyclines and trimethoprim/sulfamethoxazole.
1.3 Community-Acquired Pneumonia: 5-day Treatment Regimen
Levofloxacin tablets are indicated for the treatment of community-acquired pneumonia due to Streptococcus pneumoniae (excluding multi-drug-resistant strains [MDRSP]), Haemophilus influenzae, Haemophilus parainfluenzae, Mycoplasma pneumoniae, or Chlamydophila pneumoniae [see Dosage and Administration (2.1) and Clinical Studies (14.3)].
1.4 Acute Bacterial Sinusitis: 5-day and 10-14 day Treatment Regimens
Levofloxacin tablets are indicated for the treatment of acute bacterial sinusitis due to Streptococcus pneumoniae, Haemophilus influenzae, or Moraxella catarrhalis [see Clinical Studies (14.4)].
1.5 Acute Bacterial Exacerbation of Chronic Bronchitis
Levofloxacin tablets are indicated for the treatment of acute bacterial exacerbation of chronic bronchitis due to methicillin-susceptible Staphylococcus aureus, Streptococcus pneumoniae, Haemophilus influenzae, Haemophilus parainfluenzae, or Moraxella catarrhalis.
1.6 Complicated Skin and Skin Structure Infections
Levofloxacin tablets are indicated for the treatment of complicated skin and skin structure infections due to methicillin-susceptible Staphylococcus aureus, Enterococcus faecalis, Streptococcus pyogenes, or Proteus mirabilis [see Clinical Studies (14.5)].
1.7 Uncomplicated Skin and Skin Structure Infections
Levofloxacin tablets are indicated for the treatment of uncomplicated skin and skin structure infections (mild to moderate) including abscesses, cellulitis, furuncles, impetigo, pyoderma, wound infections, due to methicillin-susceptible Staphylococcus aureus, or Streptococcus pyogenes.
1.8 Chronic Bacterial Prostatitis
Levofloxacin tablets are indicated for the treatment of chronic bacterial prostatitis due to Escherichia coli, Enterococcus faecalis, or methicillin-susceptible Staphylococcus epidermidis [see Clinical Studies (14.6)].
1.9 Complicated Urinary Tract Infections: 5-day Treatment Regimen
Levofloxacin tablets are indicated for the treatment of complicated urinary tract infections due to Escherichia coli, Klebsiella pneumoniae, or Proteus mirabilis [see Clinical Studies (14.7)].
1.10 Complicated Urinary Tract Infections: 10-day Treatment Regimen
Levofloxacin tablets are indicated for the treatment of complicated urinary tract infections (mild to moderate) due to Enterococcus faecalis, Enterobacter cloacae, Escherichia coli, Klebsiella pneumoniae, Proteus mirabilis, or Pseudomonas aeruginosa [see Clinical Studies (14.8)].
1.11 Acute Pyelonephritis: 5 or 10-day Treatment Regimen
Levofloxacin tablets are indicated for the treatment of acute pyelonephritis caused by Escherichia coli, including cases with concurrent bacteremia [see Clinical Studies (14.7, 14.8)].
1.12 Uncomplicated Urinary Tract Infections
Levofloxacin tablets are indicated for the treatment of uncomplicated urinary tract infections (mild to moderate) due to Escherichia coli, Klebsiella pneumoniae, or Staphylococcus saprophyticus.
1.13 Inhalational Anthrax (Post-Exposure)
Levofloxacin tablets are indicated for inhalational anthrax (post-exposure) to reduce the incidence or progression of disease following exposure to aerosolized Bacillus anthracis. The effectiveness of levofloxacin is based on plasma concentrations achieved in humans, a surrogate endpoint reasonably likely to predict clinical benefit. Levofloxacin tablets have not been tested in humans for the post-exposure prevention of inhalation anthrax. The safety of levofloxacin tablets in adults for durations of therapy beyond 28 days or in pediatric patients for durations of therapy beyond 14 days has not been studied. Prolonged levofloxacin therapy should only be used when the benefit outweighs the risk [see Dosage and Administration (2.1, 2.2) and Clinical Studies (14.9)].
2. DOSAGE AND ADMINISTRATION
2.1 Dosage in Adult Patients with Normal Renal Function
The usual dose of levofloxacin tablets is 250 mg, 500 mg, or 750 mg administered orally every 24 hours, as indicated by infection and described in Table 1.
These recommendations apply to patients with creatinine clearance ≥50 mL/min. For patients with creatinine clearance < 50 mL/min, adjustments to the dosing regimen are required [see Dosage and Administration (2.3)].
|
* Due to the designated pathogens [see Indications and Usage (1)]. |
||
|
†
Sequential therapy (intravenous to oral) may be instituted at the discretion of the physician. |
||
|
‡ Due to methicillin-susceptible Staphylococcus aureus, Streptococcus pneumoniae (including multi-drug-resistant strains [MDRSP]), Haemophilus influenzae, Haemophilus parainfluenzae, Klebsiella pneumoniae, Moraxella catarrhalis, Chlamydophila pneumoniae, Legionella pneumophila, or Mycoplasma pneumoniae [see Indications and Usage (1.2)]. |
||
|
§ Due to Streptococcus pneumoniae (excluding multi-drug-resistant strains [MDRSP]), Haemophilus influenzae, Haemophilus parainfluenzae, Mycoplasma pneumoniae, or Chlamydophila pneumoniae [see Indications and Usage (1.3)]. |
||
|
¶ This regimen is indicated for cUTI due to Escherichia
coli, Klebsiella
pneumoniae, Proteus
mirabilis and AP due to E
.
coli, including cases with concurrent bacteremia. |
||
|
# This regimen is indicated for cUTI due to Enterococcus
faecalis, Enterococcus
cloacae, Escherichia
coli, Klebsiella
pneumoniae, Proteus
mirabilis, Pseudomonas
aeruginosa; and for AP due to E
.
coli. |
||
|
Þ Drug administration should begin as soon as possible after suspected or confirmed exposure to aerosolized B. anthracis. This indication is based on a surrogate endpoint. Levofloxacin plasma concentrations achieved in humans are reasonably likely to predict clinical benefit [see Clinical Studies (14.9)]. |
||
|
ß The safety of levofloxacin tablets in adults for durations of therapy beyond 28 days or in pediatric patients for durations beyond 14 days has not been studied. An increased incidence of musculoskeletal adverse events compared to controls has been observed in pediatric patients [see Warnings and Precautions (5.10), Use in Specific Populations (8.4), and Clinical Studies (14.9)]. Prolonged levofloxacin therapy should only be used when the benefit outweighs the risk. |
||
|
Type
of
Infection
*
|
Dosed
Every
24
hours
|
Duration
( days )† |
| Nosocomial Pneumonia |
750 mg |
7-14 |
| Community Acquired Pneumonia‡ |
500 mg |
7-14 |
| Community Acquired Pneumonia§ |
750 mg |
5 |
| Acute Bacterial Sinusitis |
750 mg |
5 |
|
|
500 mg |
10-14 |
| Acute Bacterial Exacerbation of Chronic Bronchitis |
500 mg |
7 |
| Complicated Skin and Skin Structure Infections (SSSI) |
750 mg |
7-14 |
| Uncomplicated SSSI |
500 mg |
7-10 |
| Chronic Bacterial Prostatitis |
500 mg |
28 |
| Complicated Urinary Tract Infection (cUTI) or Acute Pyelonephritis (AP)¶ |
750 mg |
5 |
| Complicated Urinary Tract Infection (cUTI) or Acute Pyelonephritis (AP)# |
250 mg |
10 |
| Uncomplicated Urinary Tract Infection |
250 mg |
3 |
| Inhalational Anthrax (Post-Exposure), adult and pediatric patients > 50 kg and ≥ 6 months of ageÞ,ß Pediatric patients < 50 kg and ≥ 6 months of ageÞ,ß
|
500 mg see Table 2 below (2.2) |
60ß 60ß |
2.2 Dosage in Pediatric Patients
The dosage in pediatric patients ≥ 6 months of age is described below in Table 2.
|
* Due to Bacillus anthracis [see Indications and Usage (1.13)] |
|||
|
† Sequential therapy (intravenous to oral) may be instituted at the discretion of the physician. |
|||
|
‡ Drug administration should begin as soon as possible after suspected or confirmed exposure to aerosolized B. anthracis. This indication is based on a surrogate endpoint. Levofloxacin plasma concentrations achieved in humans are reasonably likely to predict clinical benefit [see Clinical Studies (14.9)] |
|||
|
§ The safety of levofloxacin tablets in pediatric patients for durations of therapy beyond 14 days has not been studied. An increased incidence of musculoskeletal adverse events compared to controls has been observed in pediatric patients [see Warnings and Precautions (5.10), Use in Specific Populations (8.4), and Clinical Studies (14.9)]. Prolonged levofloxacin therapy should only be used when the benefit outweighs the risk. |
|||
|
|
|||
|
Type
of
Infection
*
|
Dose
|
Freq
.
Once
every
|
Duration
†
|
| Inhalational Anthrax (post-exposure) ‡,§ |
|
|
|
| Pediatric patients > 50 kg and ≥ 6 months of age |
500 mg |
24 hr |
60 days§
|
|
Pediatric patients < 50 kg and ≥ 6 months of age |
8 mg/kg (not to exceed 250 mg per dose) |
12 hr |
60 days§
|
2.3 Dosage Adjustment in Adults with Renal Impairment
Administer levofloxacin tablets with caution in the presence of renal insufficiency. Careful clinical observation and appropriate laboratory studies should be performed prior to and during therapy since elimination of levofloxacin may be reduced.
No adjustment is necessary for patients with a creatinine clearance ≥ 50 mL/min.
In patients with impaired renal function (creatinine clearance < 50 mL/min), adjustment of the dosage regimen is necessary to avoid the accumulation of levofloxacin due to decreased clearance [see Use in Specific Populations (8.6)].
Table 3 shows how to adjust dose based on creatinine clearance.
|
Dosage
in
Normal Renal Function Every 24 hours |
Creatinine
Clearance 20 to 49 mL / min |
Creatinine
Clearance 10 to 19 mL / min |
Hemodialysis
or Chronic Ambulatory Peritoneal Dialysis ( CAPD ) |
| 750 mg |
750 mg every 48 hours |
750 mg initial dose, then 500 mg every 48 hours |
750 mg initial dose, then 500 mg every 48 hours |
| 500 mg |
500 mg initial dose, then 250 mg every 24 hours |
500 mg initial dose, then 250 mg every 48 hours |
500 mg initial dose, then 250 mg every 48 hours |
| 250 mg |
No dosage adjustment required |
250 mg every 48 hours. If treating uncomplicated UTI, then no dosage adjustment is required |
No information on dosing adjustment is available |
2.4 Drug Interaction With Chelation Agents: Antacids, Sucralfate, Metal Cations, Multivitamins
Levofloxacin Tablets
Levofloxacin tablets should be administered at least two hours before or two hours after antacids containing magnesium, aluminum, as well as sucralfate, metal cations such as iron, and multivitamin preparations with zinc or didanosine chewable/buffered tablets or the pediatric powder for oral solution [see Drug Interactions (7.1) and Patient Counseling Information (17.2)].
2.5 Administration Instructions
Food and Levofloxacin Tablets
Levofloxacin tablets can be administered without regard to food.
Hydration for Patients Receiving Levofloxacin Tablets
Adequate hydration of patients receiving oral levofloxacin tablets should be maintained to prevent the formation of highly concentrated urine. Crystalluria and cylindruria have been reported with quinolones [see Adverse Reactions (6.1) and Patient Counseling Information (17.2)].
3. DOSAGE FORMS AND STRENGTHS
TABLETS, Film-coated, capsule-shaped
- 250 mg light pink colored capsule-shaped film-coated tablets debossed with "250" on one side and "1082" on other side.
- 500 mg brick red colored capsule-shaped film-coated tablets debossed with "83" on one side and plain on other side.
- 750 mg white to off-white colored capsule-shaped film-coated tablets debossed with "750" on one side and "1084"on other side.
4. CONTRAINDICATIONS
Levofloxacin tablets are contraindicated in persons with known hypersensitivity to levofloxacin, or other quinolone antibacterials [see Warnings and Precautions (5.3)].
5. WARNINGS AND PRECAUTIONS
5.1 Tendinopathy and Tendon Rupture
Fluoroquinolones, including levofloxacin, are associated with an increased risk of tendinitis and tendon rupture in all ages. This adverse reaction most frequently involves the Achilles tendon, and rupture of the Achilles tendon may require surgical repair. Tendinitis and tendon rupture in the rotator cuff (the shoulder), the hand, the biceps, the thumb, and other tendon sites have also been reported. The risk of developing fluoroquinolone-associated tendinitis and tendon rupture is further increased in older patients usually over 60 years of age, in those taking corticosteroid drugs, and in patients with kidney, heart or lung transplants. Factors, in addition to age and corticosteroid use, that may independently increase the risk of tendon rupture include strenuous physical activity, renal failure, and previous tendon disorders such as rheumatoid arthritis. Tendinitis and tendon rupture have been reported in patients taking fluoroquinolones who do not have the above risk factors. Tendon rupture can occur during or after completion of therapy; cases occurring up to several months after completion of therapy have been reported. Levofloxacin should be discontinued if the patient experiences pain, swelling, inflammation or rupture of a tendon. Patients should be advised to rest at the first sign of tendinitis or tendon rupture, and to contact their healthcare provider regarding changing to a non-quinolone antimicrobial drug. [see Adverse Reactions (6.3); Patient Counseling Information (17.3)].
5.2 Exacerbation of Myasthenia Gravis
Fluoroquinolones, including levofloxacin, have neuromuscular blocking activity and may exacerbate muscle weakness in persons with myasthenia gravis. Postmarketing serious adverse events, including deaths and requirement for ventilatory support, have been associated with fluoroquinolone use in persons with myasthenia gravis. Avoid levofloxacin in patients with a known history of myasthenia gravis [see Adverse Reactions (6.3); Patient Counseling Information (17.3)].
5.3 Hypersensitivity Reactions
Serious and occasionally fatal hypersensitivity and/or anaphylactic reactions have been reported in patients receiving therapy with fluoroquinolones, including levofloxacin. These reactions often occur following the first dose. Some reactions have been accompanied by cardiovascular collapse, hypotension/shock, seizure, loss of consciousness, tingling, angioedema (including tongue, laryngeal, throat, or facial edema/swelling), airway obstruction (including bronchospasm, shortness of breath, and acute respiratory distress), dyspnea, urticaria, itching, and other serious skin reactions. Levofloxacin should be discontinued immediately at the first appearance of a skin rash or any other sign of hypersensitivity. Serious acute hypersensitivity reactions may require treatment with epinephrine and other resuscitative measures, including oxygen, intravenous fluids, antihistamines, corticosteroids, pressor amines, and airway management, as clinically indicated [see Adverse Reactions (6); Patient Counseling Information (17.3)].
5.4 Other Serious and Sometimes Fatal Reactions
Other serious and sometimes fatal events, some due to hypersensitivity, and some due to uncertain etiology, have been reported rarely in patients receiving therapy with fluoroquinolones, including levofloxacin. These events may be severe and generally occur following the administration of multiple doses. Clinical manifestations may include one or more of the following:
- fever, rash, or severe dermatologic reactions (e.g., toxic epidermal necrolysis, Stevens-Johnson Syndrome);
- vasculitis; arthralgia; myalgia; serum sickness;
- allergic pneumonitis;
- interstitial nephritis; acute renal insufficiency or failure;
- hepatitis; jaundice; acute hepatic necrosis or failure;
- anemia, including hemolytic and aplastic; thrombocytopenia, including thrombotic thrombocytopenic purpura; leukopenia; agranulocytosis; pancytopenia; and/or other hematologic abnormalities.
5.5 Hepatotoxicity
Post-marketing reports of severe hepatotoxicity (including acute hepatitis and fatal events) have been received for patients treated with levofloxacin. No evidence of serious drug-associated hepatotoxicity was detected in clinical trials of over 7,000 patients. Severe hepatotoxicity generally occurred within 14 days of initiation of therapy and most cases occurred within 6 days. Most cases of severe hepatotoxicity were not associated with hypersensitivity [see Warnings and Precautions (5.4)]. The majority of fatal hepatotoxicity reports occurred in patients 65 years of age or older and most were not associated with hypersensitivity. Levofloxacin should be discontinued immediately if the patient develops signs and symptoms of hepatitis [see Adverse Reactions (6); Patient Counseling Information (17.3)].
5.6 Central Nervous System Effects
Convulsions and toxic psychoses have been reported in patients receiving fluoroquinolones, including levofloxacin. Fluoroquinolones may also cause increased intracranial pressure and central nervous system stimulation which may lead to tremors, restlessness, anxiety, lightheadedness, confusion, hallucinations, paranoia, depression, nightmares, insomnia, and, rarely, suicidal thoughts or acts. These reactions may occur following the first dose. If these reactions occur in patients receiving levofloxacin, the drug should be discontinued and appropriate measures instituted. As with other fluoroquinolones, levofloxacin should be used with caution in patients with a known or suspected central nervous system (CNS) disorder that may predispose them to seizures or lower the seizure threshold (e.g., severe cerebral arteriosclerosis, epilepsy) or in the presence of other risk factors that may predispose them to seizures or lower the seizure threshold (e.g., certain drug therapy, renal dysfunction.) [see Adverse Reactions (6); Drug Interactions (7.4, 7.5); Patient Counseling Information (17.3)].
5.7 Clostridium difficile-Associated Diarrhea
Clostridium difficile-associated diarrhea (CDAD) has been reported with use of nearly all antibacterial agents, including levofloxacin, and may range in severity from mild diarrhea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
C. difficile produces toxins A and B which contribute to the development of CDAD. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhea following antibiotic use. Careful medical history is necessary since CDAD has been reported to occur over two months after the administration of antibacterial agents.
If CDAD is suspected or confirmed, ongoing antibiotic use not directed against C. difficile may need to be discontinued. Appropriate fluid and electrolyte management, protein supplementation, antibiotic treatment of C. difficile, and surgical evaluation should be instituted as clinically indicated [see Adverse Reactions (6.2), Patient Counseling Information (17.3)].
5.8 Peripheral Neuropathy
Rare cases of sensory or sensorimotor axonal polyneuropathy affecting small and/or large axons resulting in paresthesias, hypoesthesias, dysesthesias and weakness have been reported in patients receiving fluoroquinolones, including levofloxacin. Levofloxacin should be discontinued if the patient experiences symptoms of neuropathy including pain, burning, tingling, numbness, and/or weakness or other alterations of sensation including light touch, pain, temperature, position sense, and vibratory sensation in order to prevent the development of an irreversible condition [see Adverse Reactions (6), Patient Counseling Information (17.3)].
5.9 Prolongation of the QT Interval
Some fluoroquinolones, including levofloxacin, have been associated with prolongation of the QT interval on the electrocardiogram and infrequent cases of arrhythmia. Rare cases of torsade de pointes have been spontaneously reported during postmarketing surveillance in patients receiving fluoroquinolones, including levofloxacin. Levofloxacin should be avoided in patients with known prolongation of the QT interval, patients with uncorrected hypokalemia, and patients receiving class IA (quinidine, procainamide), or class III (amiodarone, sotalol) antiarrhythmic agents. Elderly patients may be more susceptible to drug-associated effects on the QT interval [see Adverse Reactions (6.3), Use in Specific Populations (8.5), and Patient Counseling Information (17.3)].
5.10 Musculoskeletal Disorders in Pediatric Patients and Arthropathic Effects in Animals
Levofloxacin is indicated in pediatric patients (≥6 months of age) only for the prevention of inhalational anthrax (post-exposure) [see Indications and Usage (1.13)]. An increased incidence of musculoskeletal disorders (arthralgia, arthritis, tendinopathy, and gait abnormality) compared to controls has been observed in pediatric patients receiving levofloxacin [see Use in Specific Populations (8.4)].
In immature rats and dogs, the oral and intravenous administration of levofloxacin resulted in increased osteochondrosis. Histopathological examination of the weight-bearing joints of immature dogs dosed with levofloxacin revealed persistent lesions of the cartilage. Other fluoroquinolones also produce similar erosions in the weight-bearing joints and other signs of arthropathy in immature animals of various species [see Animal Toxicology and/or Pharmacology (13.2)].
5.11 Blood Glucose Disturbances
As with other fluoroquinolones, disturbances of blood glucose, including symptomatic hyper- and hypoglycemia, have been reported with levofloxacin, usually in diabetic patients receiving concomitant treatment with an oral hypoglycemic agent (e.g., glyburide) or with insulin. In these patients, careful monitoring of blood glucose is recommended. If a hypoglycemic reaction occurs in a patient being treated with levofloxacin, levofloxacin should be discontinued and appropriate therapy should be initiated immediately [see Adverse Reactions (6.2); Drug Interactions (7.3); Patient Counseling Information (17.4)].
5.12 Photosensitivity/Phototoxicity
Moderate to severe photosensitivity/phototoxicity reactions, the latter of which may manifest as exaggerated sunburn reactions (e.g., burning, erythema, exudation, vesicles, blistering, edema) involving areas exposed to light (typically the face, "V" area of the neck, extensor surfaces of the forearms, dorsa of the hands), can be associated with the use of fluoroquinolones after sun or UV light exposure. Therefore, excessive exposure to these sources of light should be avoided. Drug therapy should be discontinued if photosensitivity/phototoxicity occurs [see Adverse Reactions (6.3); Patient Counseling Information (17.3)].
5.13 Development of Drug Resistant Bacteria
Prescribing levofloxacin in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria [see Patient Counseling Information (17.1)].
6. ADVERSE REACTIONS
6.1 Serious and Otherwise Important Side Effects
The following serious and otherwise important adverse drug reactions are discussed in greater detail in other sections of labeling:
- Tendon Effects [see Warnings and Precautions (5.1)]
- Exacerbation of Myasthenia Gravis [see Warnings and Precautions (5.2)]
- Hypersensitivity Reactions [see Warnings and Precautions (5.3)]
- Other Serious and Sometimes Fatal Reactions [see Warnings and Precautions (5.4)]
- Hepatotoxicity [see Warnings and Precautions (5.5)]
- Central Nervous System Effects [see Warnings and Precautions (5.6)]
- Clostridium difficile-Associated Diarrhea [see Warnings and Precautions (5.7)]
- Peripheral Neuropathy [see Warnings and Precautions (5.8)]
- Prolongation of the QT Interval [see Warnings and Precautions (5.9)]
- Musculoskeletal Disorders in Pediatric Patients [see Warnings and Precautions (5.10)]
- Blood Glucose Disturbances [see Warnings and Precautions (5.11)]
- Photosensitivity/Phototoxicity [see Warnings and Precautions (5.12)]
- Development of Drug Resistant Bacteria [see Warnings and Precautions (5.13)]
Crystalluria and cylindruria have been reported with quinolones, including levofloxacin. Therefore, adequate hydration of patients receiving levofloxacin should be maintained to prevent the formation of a highly concentrated urine [see Dosage and Administration (2.5)].
6.2 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The data described below reflect exposure to levofloxacin in 7537 patients in 29 pooled Phase 3 clinical trials. The population studied had a mean age of 50 years (approximately 74% of the population was < 65 years of age), 50% were male, 71% were Caucasian, 19% were Black. Patients were treated with levofloxacin for a wide variety of infectious diseases [see Indications and Usage (1)]. Patients received levofloxacin doses of 750 mg once daily, 250 mg once daily, or 500 mg once or twice daily. Treatment duration was usually 3-14 days, and the mean number of days on therapy was 10 days.
The overall incidence, type and distribution of adverse reactions was similar in patients receiving levofloxacin tablets doses of 750 mg once daily, 250 mg once daily, and 500 mg once or twice daily. Discontinuation of levofloxacin due to adverse drug reactions occurred in 4.3% of patients overall, 3.8% of patients treated with the 250 mg and 500 mg doses and 5.4% of patients treated with the 750 mg dose. The most common adverse drug reactions leading to discontinuation with the 250 and 500 mg doses were gastrointestinal (1.4%), primarily nausea (0.6%); vomiting (0.4%); dizziness (0.3%); and headache (0.2%). The most common adverse drug reactions leading to discontinuation with the 750 mg dose were gastrointestinal (1.2%), primarily nausea (0.6%), vomiting (0.5%); dizziness (0.3%); and headache (0.3%).
Adverse reactions occurring in ≥1% of levofloxacin-treated patients and less common adverse reactions, occurring in 0.1 to <1% of levofloxacin-treated patients, are shown in Table 4 and Table 5, respectively. The most common adverse drug reactions (≥3%) are nausea, headache, diarrhea, insomnia, constipation, and dizziness.
|
* N = 7274 |
||
|
† N = 3758 (women) |
||
|
System
/
Organ
Class
|
Adverse
Reaction
|
%
( N = 7537 ) |
|
Infections
and
Infestations
|
moniliasis |
1 |
|
Psychiatric
Disorders
|
insomnia*[see
Warnings
and
Precautions ( 5 . 6 )] |
4 |
|
Nervous
System
Disorders
|
headache dizziness [ see Warnings and Precautions ( 5 . 6 )] |
6 3 |
|
Respiratory, Thoracic
and
Mediastinal Disorders |
dyspnea [
see
Warnings
and
Precautions
( 5 . 3 )] |
1 |
|
Gastrointestinal
Disorders
|
nausea diarrhea constipation abdominal pain vomiting dyspepsia |
7 5 3 2 2 2 |
|
Skin
and
Subcutaneous
Tissue Disorders |
rash [
see
Warnings
and
Precautions
(
5
.
3
)]
pruritus |
2 1 |
|
Reproductive
System
and
Breast Disorders |
vaginitis |
1†
|
|
General
Disorders
and
Administration
Site
Conditions
|
edema injection site reaction chest pain |
1 1 1 |
|
*N = 7274 |
|
|
System
/
Organ
Class
|
Adverse
Reaction
|
|
Infections
and
Infestations
|
genital moniliasis |
|
Blood
and
Lymphatic
System Disorders |
anemia thrombocytopenia granulocytopenia [ see Warnings and Precautions ( 5 . 4 )] |
|
Immune
System
Disorders
|
allergic reaction [ see Warnings and Precautions ( 5 . 3, 5 . 4 )] |
|
Metabolism
and
Nutrition
Disorders |
hyperglycemia hypoglycemia [ see Warnings and Precautions ( 5 . 11 )] hyperkalemia |
|
Psychiatric
Disorders
|
anxiety agitation confusion depression hallucination nightmare* [ see Warnings and Precautions ( 5 . 6 )] sleep disorder* anorexia abnormal dreaming* |
|
Nervous
System
Disorders
|
tremor convulsions [ see Warnings and Precautions ( 5 . 6 )] paresthesia [ see Warnings and Precautions ( 5 . 8 )] vertigo hypertonia hyperkinesias abnormal gait somnolence*syncope |
|
Respiratory, Thoracic
and
Mediastinal Disorders |
epistaxis |
|
Cardiac Disorders |
cardiac arrest palpitation ventricular tachycardia ventricular arrhythmia |
|
Vascular
Disorders
|
phlebitis |
|
Gastrointestinal
Disorders
|
gastritis stomatitis pancreatitis esophagitis gastroenteritis glossitis pseudomembraneous/ C . difficile colitis [ see Warnings and Precautions ( 5 . 7 )] |
|
Hepatobiliary
Disorders
|
abnormal hepatic function increased hepatic enzymes increased alkaline phosphatase |
|
Skin
and
Subcutaneous
Tissue Disorders |
urticaria [
see
Warnings
and
Precautions
(
5
.
3
)]
|
|
Musculoskeletal
and
Connective Tissue Disorders |
arthralgia tendinitis [ see Warnings and Precautions ( 5 . 1 )] myalgia skeletal pain |
|
Renal
and
Urinary
Disorders
|
abnormal renal function acute renal failure [ see Warnings and Precautions ( 5 . 4 )] |
In clinical trials using multiple-dose therapy, ophthalmologic abnormalities, including cataracts and multiple punctate lenticular opacities, have been noted in patients undergoing treatment with quinolones, including levofloxacin. The relationship of the drugs to these events is not presently established.
6.3 Postmarketing Experience
Table 6 lists adverse reactions that have been identified during post-approval use of levofloxacin. Because these reactions are reported voluntarily from a population of uncertain size, reliably estimating their frequency or establishing a causal relationship to drug exposure is not always possible.
|
System
/
Organ
Class
|
Adverse
Reaction
|
|
Blood
and
Lymphatic
System
Disorders
|
pancytopenia aplastic anemia leukopenia hemolytic anemia [see Warnings and Precautions (5.4)] eosinophilia |
|
Immune
System
Disorders
|
hypersensitivity reactions, sometimes fatal including: anaphylactic/anaphylactoid reactions anaphylactic shock angioneurotic edema serum sickness [see Warnings and Precautions (5.3, 5.4)] |
|
Psychiatric
Disorders
|
psychosis paranoia isolated reports of suicide attempt and suicidal ideation [see Warnings and Precautions (5.6)] |
|
Nervous
System
Disorders
|
exacerbation of myasthenia gravis [see Warnings and Precautions (5.2)] anosmia ageusia parosmia dysgeusia peripheral neuropathy [see Warnings and Precautions (5.8)] isolated reports of encephalopathy abnormal electroencephalogram (EEG) dysphonia |
|
Eye
Disorders
|
vision disturbance, including diplopia visual acuity reduced vision blurred scotoma |
|
Ear
and
Labyrinth
Disorders
|
hypoacusis tinnitus |
|
Cardiac
Disorders
|
isolated reports of torsade de pointes electrocardiogram QT prolonged [see Warnings and Precautions (5.9)] tachycardia |
|
Vascular
Disorders
|
vasodilatation |
|
Respiratory, Thoracic
and
Mediastinal Disorders |
isolated reports of allergic pneumonitis [see Warnings and Precautions (5.4)] |
|
Hepatobiliary
Disorders
|
hepatic failure (including fatal cases) hepatitis jaundice [see Warnings and Precautions (5.4, 5.5)] |
|
Skin
and
Subcutaneous
Tissue Disorders |
bullous eruptions to include: Stevens-Johnson Syndrome toxic epidermal necrolysis erythema multiforme [see Warnings and Precautions (5.4)] photosensitivity/phototoxicity reaction [see Warnings and Precautions (5.12)] leukocytoclastic vasculitis |
|
Musculoskeletal
and
Connective Tissue Disorders |
tendon rupture [see Warnings and Precautions (5.1)] muscle injury, including rupture rhabdomyolysis |
|
Renal
and
Urinary
Disorders
|
interstitial nephritis [see Warnings and Precautions (5.4)] |
|
General
Disorders
and
Administration Site Conditions |
multi-organ failure pyrexia |
|
Investigations
|
prothrombin time prolonged international normalized ratio prolonged muscle enzymes increased |
7. DRUG INTERACTIONS
7.1 Chelation Agents: Antacids, Sucralfate, Metal Cations, Multivitamins
Levofloxacin Tablets
While the chelation by divalent cations is less marked than with other fluoroquinolones, concurrent administration of levofloxacin tablets with antacids containing magnesium, or aluminum, as well as sucralfate, metal cations such as iron, and multivitamin preparations with zinc may interfere with the gastrointestinal absorption of levofloxacin, resulting in systemic levels considerably lower than desired. Tablets with antacids containing magnesium, aluminum, as well as sucralfate, metal cations such as iron, and multivitamins preparations with zinc or didanosine may substantially interfere with the gastrointestinal absorption of levofloxacin, resulting in systemic levels considerably lower than desired. These agents should be taken at least two hours before or two hours after oral levofloxacin tablet administration.
7.2 Warfarin
No significant effect of levofloxacin on the peak plasma concentrations, AUC, and other disposition parameters for R- and S- warfarin was detected in a clinical study involving healthy volunteers. Similarly, no apparent effect of warfarin on levofloxacin absorption and disposition was observed. However, there have been reports during the postmarketing experience in patients that levofloxacin enhances the effects of warfarin. Elevations of the prothrombin time in the setting of concurrent warfarin and levofloxacin use have been associated with episodes of bleeding. Prothrombin time, International Normalized Ratio (INR), or other suitable anticoagulation tests should be closely monitored if levofloxacin is administered concomitantly with warfarin. Patients should also be monitored for evidence of bleeding [see Adverse Reactions (6.3); Patient Counseling Information (17.4)].
7.3 Antidiabetic Agents
Disturbances of blood glucose, including hyperglycemia and hypoglycemia, have been reported in patients treated concomitantly with fluoroquinolones and an antidiabetic agent. Therefore, careful monitoring of blood glucose is recommended when these agents are co-administered [see Warnings and Precautions (5.11); Adverse Reactions (6.2), Patient Counseling Information (17.4)].
7.4 Non-Steroidal Anti-Inflammatory Drugs
The concomitant administration of a non-steroidal anti-inflammatory drug with a fluoroquinolone, including levofloxacin, may increase the risk of CNS stimulation and convulsive seizures [see Warnings and Precautions (5.6)].
7.5 Theophylline
No significant effect of levofloxacin on the plasma concentrations, AUC, and other disposition parameters for theophylline was detected in a clinical study involving healthy volunteers. Similarly, no apparent effect of theophylline on levofloxacin absorption and disposition was observed. However, concomitant administration of other fluoroquinolones with theophylline has resulted in prolonged elimination half-life, elevated serum theophylline levels, and a subsequent increase in the risk of theophylline-related adverse reactions in the patient population. Therefore, theophylline levels should be closely monitored and appropriate dosage adjustments made when levofloxacin is co-administered. Adverse reactions, including seizures, may occur with or without an elevation in serum theophylline levels [see Warnings and Precautions (5.6)].
7.6 Cyclosporine
No significant effect of levofloxacin on the peak plasma concentrations, AUC, and other disposition parameters for cyclosporine was detected in a clinical study involving healthy volunteers. However, elevated serum levels of cyclosporine have been reported in the patient population when co-administered with some other fluoroquinolones. Levofloxacin Cmax and ke were slightly lower while Tmax and t1/2 were slightly longer in the presence of cyclosporine than those observed in other studies without concomitant medication. The differences, however, are not considered to be clinically significant. Therefore, no dosage adjustment is required for levofloxacin or cyclosporine when administered concomitantly.
7.7 Digoxin
No significant effect of levofloxacin on the peak plasma concentrations, AUC, and other disposition parameters for digoxin was detected in a clinical study involving healthy volunteers. Levofloxacin absorption and disposition kinetics were similar in the presence or absence of digoxin. Therefore, no dosage adjustment for levofloxacin or digoxin is required when administered concomitantly.
7.8 Probenecid and Cimetidine
No significant effect of probenecid or cimetidine on the Cmax of levofloxacin was observed in a clinical study involving healthy volunteers. The AUC and t1/2 of levofloxacin were higher while CL/F and CLR were lower during concomitant treatment of levofloxacin with probenecid or cimetidine compared to levofloxacin alone. However, these changes do not warrant dosage adjustment for levofloxacin when probenecid or cimetidine is co-administered.
7.9 Interactions with Laboratory or Diagnostic Testing
Some fluoroquinolones, including levofloxacin, may produce false-positive urine screening results for opiates using commercially available immunoassay kits. Confirmation of positive opiate screens by more specific methods may be necessary.
8. USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Pregnancy Category C. Levofloxacin was not teratogenic in rats at oral doses as high as 810 mg/kg/day which corresponds to 9.4 times the highest recommended human dose based upon relative body surface area, or at intravenous doses as high as 160 mg/kg/day corresponding to 1.9 times the highest recommended human dose based upon relative body surface area. The oral dose of 810 mg/kg/day to rats caused decreased fetal body weight and increased fetal mortality. No teratogenicity was observed when rabbits were dosed orally as high as 50 mg/kg/day which corresponds to 1.1 times the highest recommended human dose based upon relative body surface area, or when dosed intravenously as high as 25 mg/kg/day, corresponding to 0.5 times the highest recommended human dose based upon relative body surface area.
There are, however, no adequate and well-controlled studies in pregnant women. Levofloxacin should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
8.3 Nursing Mothers
Based on data on other fluoroquinolones and very limited data on levofloxacin, it can be presumed that levofloxacin will be excreted in human milk. Because of the potential for serious adverse reactions from levofloxacin in nursing infants, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
8.4 Pediatric Use
Quinolones, including levofloxacin, cause arthropathy and osteochondrosis in juvenile animals of several species. [see Warnings and Precautions (5.10) and Animal Toxicology and/or Pharmacology (13.2)].
Inhalational Anthrax (Post-Exposure)
Levofloxacin is indicated in pediatric patients for inhalational anthrax (post-exposure). The risk-benefit assessment indicates that administration of levofloxacin to pediatric patients is appropriate. The safety of levofloxacin in pediatric patients treated for more than 14 days has not been studied. Pediatric patients cleared levofloxacin faster than adult patients resulting in lower plasma exposures than adults for a given mg/kg dose [see Indications and Usage (1.13), Dosage and Administration (2.2), Clinical Pharmacology (12.3) and Clinical Studies (14.9)].
Adverse Events
In clinical trials, 1534 children (6 months to 16 years of age) were treated with oral and intravenous levofloxacin. Children 6 months to 5 years of age received levofloxacin 10 mg/kg twice a day and children greater than 5 years of age received 10 mg/kg once a day (maximum 500 mg per day) for approximately 10 days.
A subset of children in the clinical trials (1340 levofloxacin-treated and 893 non-fluoroquinolone-treated) enrolled in a prospective, long-term surveillance study to assess the incidence of protocol-defined musculoskeletal disorders (arthralgia, arthritis, tendinopathy, gait abnormality) during 60 days and 1 year following the first dose of the study drug. Children treated with levofloxacin had a significantly higher incidence of musculoskeletal disorders when compared to the non-fluoroquinolone-treated children as illustrated in Table 7.
|
* Non-Fluoroquinolone: ceftriaxone, amoxicillin/clavulanate, clarithromycin |
|||
|
† 2-sided Fisher’s Exact Test |
|||
|
‡ There were 1199 levofloxacin-treated and 804 non-fluoroquinolone-treated children who had a one-year evaluation visit. However, the incidence of musculoskeletal disorders was calculated using all reported events during the specified period for all children enrolled regardless of whether they completed the 1-year evaluation visit. |
|||
| Follow - up Period | Levofloxacin N = 1340 | Non - Fluoroquinolone * N = 893 | p - value † |
| 60 days | 28 (2.1%) | 8 (0.9%) | p = 0.038 |
| 1 year ‡ | 46 (3.4%) | 16 (1.8%) | p = 0.025 |
Arthralgia was the most frequently occurring musculoskeletal disorder in both treatment groups. Most of the musculoskeletal disorders in both groups involved multiple weight-bearing joints. Disorders were moderate in 8/46 (17%) children and mild in 35/46 (76%) levofloxacin-treated children and most were treated with analgesics. The median time to resolution was 7 days for levofloxacin-treated children and 9 for non-fluoroquinolone-treated children (approximately 80% resolved within 2 months in both groups). No child had a severe or serious disorder and all musculoskeletal disorders resolved without sequelae.
Vomiting and diarrhea were the most frequently reported adverse events, occurring in similar frequency in the levofloxacin-treated and non-fluoroquinolone-treated children.
In addition to the events reported in pediatric patients in clinical trials, events reported in adults during clinical trials or post-marketing experience [see Adverse Reactions (6)] may also be expected to occur in pediatric patients.
8.5 Geriatric Use
Geriatric patients are at increased risk for developing severe tendon disorders including tendon rupture when being treated with a fluoroquinolone such as levofloxacin. This risk is further increased in patients receiving concomitant corticosteroid therapy. Tendinitis or tendon rupture can involve the Achilles, hand, shoulder, or other tendon sites and can occur during or after completion of therapy; cases occurring up to several months after fluoroquinolone treatment have been reported. Caution should be used when prescribing levofloxacin to elderly patients especially those on corticosteroids. Patients should be informed of this potential side effect and advised to discontinue levofloxacin and contact their healthcare provider if any symptoms of tendinitis or tendon rupture occur [see Boxed Warning; Warnings and Precautions (5.1); and Adverse Reactions (6.3)].
In phase 3 clinical trials, 1,945 levofloxacin-treated patients (26%) were ≥ 65 years of age. Of these, 1,081 patients (14%) were between the ages of 65 and 74 and 864 patients (12%) were 75 years or older. No overall differences in safety or effectiveness were observed between these subjects and younger subjects, but greater sensitivity of some older individuals cannot be ruled out.
Severe, and sometimes fatal, cases of hepatotoxicity have been reported post-marketing in association with levofloxacin. The majority of fatal hepatotoxicity reports occurred in patients 65 years of age or older and most were not associated with hypersensitivity. Levofloxacin should be discontinued immediately if the patient develops signs and symptoms of hepatitis [see Warnings and Precautions (5.5)].
Elderly patients may be more susceptible to drug-associated effects on the QT interval. Therefore, precaution should be taken when using levofloxacin with concomitant drugs that can result in prolongation of the QT interval (e.g., class IA or class III antiarrhythmics) or in patients with risk factors for torsade de pointes (e.g., known QT prolongation, uncorrected hypokalemia) [see Warnings and Precautions (5.9)].
The pharmacokinetic properties of levofloxacin in younger adults and elderly adults do not differ significantly when creatinine clearance is taken into consideration. However, since the drug is known to be substantially excreted by the kidney, the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function [see Clinical Pharmacology (12.3)].
8.6 Renal Impairment
Clearance of levofloxacin is substantially reduced and plasma elimination half-life is substantially prolonged in patients with impaired renal function (creatinine clearance < 50 mL/min), requiring dosage adjustment in such patients to avoid accumulation. Neither hemodialysis nor continuous ambulatory peritoneal dialysis (CAPD) is effective in removal of levofloxacin from the body, indicating that supplemental doses of levofloxacin are not required following hemodialysis or CAPD [see Dosage and Administration (2.3)].
8.7 Hepatic Impairment
Pharmacokinetic studies in hepatically impaired patients have not been conducted. Due to the limited extent of levofloxacin metabolism, the pharmacokinetics of levofloxacin are not expected to be affected by hepatic impairment.
10. OVERDOSAGE
11. DESCRIPTION
12. CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Levofloxacin is a member of the fluoroquinolone class of antibacterial agents [see Clinical Pharmacology (12.4)].
12.3 Pharmacokinetics
The mean ±SD pharmacokinetic parameters of levofloxacin determined under single and steady-state conditions following oral tablet, oral solution, or intravenous (IV) doses of levofloxacin are summarized in Table 8.
|
1 clearance/bioavailability |
|||||||
|
2 volume of distribution/bioavailability |
|||||||
|
3 healthy males 18-53 years of age |
|||||||
|
4 60 min infusion for 250 mg and 500 mg doses, 90 min infusion for 750 mg dose |
|||||||
|
5 healthy male and female subjects 18-54 years of age |
|||||||
|
6 500 mg every 48h for patients with moderate renal impairment (CLCR 20-50 mL/min) and infections of the respiratory tract or skin |
|||||||
|
7 dose-normalized values (to 500 mg dose), estimated by population pharmacokinetic modeling |
|||||||
|
8 healthy males 22-75 years of age |
|||||||
|
9 healthy females 18-80 years of age |
|||||||
|
1
0 young healthy male and female subjects 18-36 years of age |
|||||||
|
1
1 healthy elderly male and female subjects 66-80 years of age |
|||||||
|
1
2 healthy males and females 19-55 years of age. |
|||||||
|
* Absolute bioavailability; F=0.99 ± 0.08 from a 500 mg tablet and F=0.99 ± 0.06 from a |
|||||||
|
750 mg tablet; |
|||||||
|
ND=not determined. |
|||||||
|
Regimen
|
Cm
a
x
( mcg / mL ) |
Tm
a
x
( h ) |
AUC
( mcg • h / mL ) |
CL
/
F1
( mL / min ) |
Vd
/
F2
( L ) |
t1
/
2
( h ) |
CLR
(
mL
/
min
)
|
|
Single
dose
|
|||||||
| 250 mg oral tablet3
|
2.8 ± 0.4 |
1.6 ± 1.0 |
27.2 ± 3.9 |
156 ± 20 |
ND |
7.3 ± 0.9 |
142 ± 21 |
| 500 mg oral tablet3* |
5.1 ± 0.8 |
1.3 ± 0.6 |
47.9 ± 6.8 |
178 ± 28 |
ND |
6.3 ± 0.6 |
103 ± 30 |
| 500 mg oral solution1
2 |
5.8 ± 1.8 |
0.8 ± 0.7 |
47.8 ± 10.8 |
183 ± 40 |
112 ± 37.2 |
7.0 ± 1.4 |
ND |
| 500 mg IV3
|
6.2 ± 1.0 |
1.0 ± 0.1 |
48.3 ± 5.4 |
175 ± 20 |
90 ± 11 |
6.4 ± 0.7 |
112 ± 25 |
| 750 mg oral tablet5* |
9.3 ± 1.6 |
1.6 ± 0.8 |
101 ± 20 |
129 ± 24 |
83 ± 17 |
7.5 ± 0.9 |
ND |
| 750 mg IV5
|
11.5 ± 4.04
|
ND |
110 ± 40 |
126 ± 39 |
75 ± 13 |
7.5 ± 1.6 |
ND |
|
Multiple
dose
|
|||||||
| 500 mg every 24h oral tablet3 |
5.7 ± 1.4 |
1.1 ± 0.4 |
47.5 ± 6.7 |
175 ± 25 |
102 ± 22 |
7.6 ± 1.6 |
116 ± 31 |
| 500 mg every 24h IV3 |
6.4 ± 0.8 |
ND |
54.6 ± 11.1 |
158 ± 29 |
91 ± 12 |
7.0 ± 0.8 |
99 ± 28 |
| 500 mg or 250 mg every 24h IV, patients with bacterial infection6 |
8.7 ± 4.07
|
ND |
72.5 ± 51.27
|
154 ± 72 |
111 ± 58 |
ND |
ND |
| 750 mg every 24h oral tablet5 |
8.6 ± 1.9 |
1.4 ± 0.5 |
90.7 ± 17.6 |
143 ± 29 |
100 ± 16 |
8.8 ± 1.5 |
116 ± 28 |
| 750 mg every 24h IV5 |
12.1 ± 4.14 |
ND |
108 ± 34 |
126 ± 37 |
80 ± 27 |
7.9 ± 1.9 |
ND |
|
500
mg
oral
tablet
single
dose, effects
of
gender
and
age
:
|
|||||||
| Male8
|
5.5 ± 1.1 |
1.2 ± 0.4 |
54.4 ± 18.9 |
166 ± 44 |
89 ± 13 |
7.5 ± 2.1 |
126 ± 38 |
| Female9 |
7.0 ± 1.6 |
1.7 ± 0.5 |
67.7 ± 24.2 |
136 ± 44 |
62 ± 16 |
6.1 ± 0.8 |
106 ± 40 |
| Young1
0
|
5.5 ± 1.0 |
1.5 ± 0.6 |
47.5 ± 9.8 |
182 ± 35 |
83 ± 18 |
6.0 ± 0.9 |
140 ± 33 |
| Elderly1
1
|
7.0 ± 1.6 |
1.4 ± 0.5 |
74.7 ± 23.3 |
121 ± 33 |
67 ± 19 |
7.6 ± 2.0 |
91 ± 29 |
|
500
mg
oral
single
dose
tablet, patients
with
renal
insufficiency
:
|
|||||||
| CLCR 50-80 mL/min |
7.5 ± 1.8 |
1.5 ± 0.5 |
95.6 ± 11.8 |
88 ± 10 |
ND |
9.1 ± 0.9 |
57 ± 8 |
| CLCR 20-49 mL/min |
7.1 ± 3.1 |
2.1 ± 1.3 |
182.1 ± 62.6 |
51 ± 19 |
ND |
27 ± 10 |
26 ± 13 |
| CLCR <20 mL/min |
8.2 ± 2.6 |
1.1 ± 1.0 |
263.5 ± 72.5 |
33 ± 8 |
ND |
35 ± 5
|
13 ± 3 |
| Hemodialysis |
5.7 ± 1.0 |
2.8 ± 2.2 |
ND |
ND |
ND |
76 ± 42 |
ND |
| CAPD |
6.9 ± 2.3 |
1.4 ± 1.1 |
ND |
ND |
ND |
51 ± 24 |
ND |
Absorption
Levofloxacin is rapidly and essentially completely absorbed after oral administration. Peak plasma concentrations are usually attained one to two hours after oral dosing. The absolute bioavailability of levofloxacin from a 500 mg tablet and a 750 mg tablet of levofloxacin are both approximately 99%, demonstrating complete oral absorption of levofloxacin. Following a single intravenous dose of levofloxacin to healthy volunteers, the mean ±SD peak plasma concentration attained was 6.2 ±1.0 mcg/mL after a 500 mg dose infused over 60 minutes and 11.5 ±4.0 mcg/mL after a 750 mg dose infused over 90 minutes. Levofloxacin Oral Solution and Tablet formulations are bioequivalent.
Levofloxacin pharmacokinetics are linear and predictable after single and multiple oral or IV dosing regimens. Steady-state conditions are reached within 48 hours following a 500 mg or 750 mg once-daily dosage regimen. The mean ±SD peak and trough plasma concentrations attained following multiple once-daily oral dosage regimens were approximately 5.7 ±1.4 and 0.5 ±0.2 mcg/mL after the 500 mg doses, and 8.6 ±1.9 and 1.1 ±0.4 mcg/mL after the 750 mg doses, respectively. The mean ±SD peak and trough plasma concentrations attained following multiple once-daily IV regimens were approximately 6.4 ±0.8 and 0.6 ±0.2 mcg/mL after the 500 mg doses, and 12.1 ±4.1 and 1.3 ±0.71 mcg/mL after the 750 mg doses, respectively. Oral administration of a 500 mg dose of levofloxacin with food prolongs the time to peak concentration by approximately 1 hour and decreases the peak concentration by approximately 14% following tablet and approximately 25% following oral solution administration. Therefore, levofloxacin tablets can be administered without regard to food.
The plasma concentration profile of levofloxacin after IV administration is similar and comparable in extent of exposure (AUC) to that observed for levofloxacin tablets when equal doses (mg/mg) are administered. Therefore, the oral and IV routes of administration can be considered interchangeable (see Figure 2 and Figure 3).
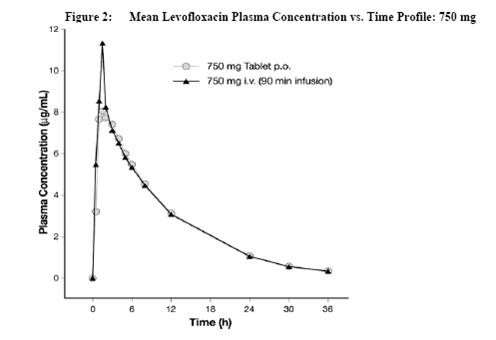
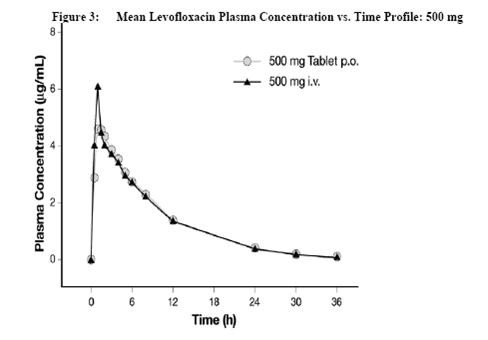
Distribution
The mean volume of distribution of levofloxacin generally ranges from 74 to 112 L after single and multiple 500 mg or 750 mg doses, indicating widespread distribution into body tissues. Levofloxacin reaches its peak levels in skin tissues and in blister fluid of healthy subjects at approximately 3 hours after dosing. The skin tissue biopsy to plasma AUC ratio is approximately 2 and the blister fluid to plasma AUC ratio is approximately 1 following multiple once-daily oral administration of 750 mg and 500 mg doses of levofloxacin, respectively, to healthy subjects. Levofloxacin also penetrates well into lung tissues. Lung tissue concentrations were generally 2- to 5- fold higher than plasma concentrations and ranged from approximately 2.4 to 11.3 mcg/g over a 24-hour period after a single 500 mg oral dose.
In vitro, over a clinically relevant range (1 to 10 mcg/mL) of serum/plasma levofloxacin concentrations, levofloxacin is approximately 24 to 38% bound to serum proteins across all species studied, as determined by the equilibrium dialysis method. Levofloxacin is mainly bound to serum albumin in humans. Levofloxacin binding to serum proteins is independent of the drug concentration.
Metabolism
Levofloxacin is stereochemically stable in plasma and urine and does not invert metabolically to its enantiomer, D-ofloxacin. Levofloxacin undergoes limited metabolism in humans and is primarily excreted as unchanged drug in the urine. Following oral administration, approximately 87% of an administered dose was recovered as unchanged drug in urine within 48 hours, whereas less than 4% of the dose was recovered in feces in 72 hours. Less than 5% of an administered dose was recovered in the urine as the desmethyl and N-oxide metabolites, the only metabolites identified in humans. These metabolites have little relevant pharmacological activity.
Excretion
Levofloxacin is excreted largely as unchanged drug in the urine. The mean terminal plasma elimination half-life of levofloxacin ranges from approximately 6 to 8 hours following single or multiple doses of levofloxacin given orally or intravenously. The mean apparent total body clearance and renal clearance range from approximately 144 to 226 mL/min and 96 to 142 mL/min, respectively. Renal clearance in excess of the glomerular filtration rate suggests that tubular secretion of levofloxacin occurs in addition to its glomerular filtration. Concomitant administration of either cimetidine or probenecid results in approximately 24% and 35% reduction in the levofloxacin renal clearance, respectively, indicating that secretion of levofloxacin occurs in the renal proximal tubule. No levofloxacin crystals were found in any of the urine samples freshly collected from subjects receiving levofloxacin.
Geriatric
There are no significant differences in levofloxacin pharmacokinetics between young and elderly subjects when the subjects’ differences in creatinine clearance are taken into consideration. Following a 500 mg oral dose of levofloxacin tablets to healthy elderly subjects (66 - 80 years of age), the mean terminal plasma elimination half-life of levofloxacin was about 7.6 hours, as compared to approximately 6 hours in younger adults. The difference was attributable to the variation in renal function status of the subjects and was not believed to be clinically significant. Drug absorption appears to be unaffected by age. Levofloxacin dose adjustment based on age alone is not necessary [see Use in Specific Populations (8.5)].
Pediatrics
The pharmacokinetics of levofloxacin following a single 7 mg/kg intravenous dose were investigated in pediatric patients ranging in age from 6 months to 16 years. Pediatric patients cleared levofloxacin faster than adult patients, resulting in lower plasma exposures than adults for a given mg/kg dose. Subsequent pharmacokinetic analyses predicted that a dosage regimen of 8 mg/kg every 12 hours (not to exceed 250 mg per dose) for pediatric patients 6 months to 17 years of age would achieve comparable steady state plasma exposures (AUC0-24 and Cmax) to those observed in adult patients administered 500 mg of levofloxacin once every 24 hours.
Gender
There are no significant differences in levofloxacin pharmacokinetics between male and female subjects when subjects’ differences in creatinine clearance are taken into consideration. Following a 500 mg oral dose of levofloxacin to healthy male subjects, the mean terminal plasma elimination half-life of levofloxacin was about 7.5 hours, as compared to approximately 6.1 hours in female subjects. This difference was attributable to the variation in renal function status of the male and female subjects and was not believed to be clinically significant. Drug absorption appears to be unaffected by the gender of the subjects. Dose adjustment based on gender alone is not necessary.
Race
The effect of race on levofloxacin pharmacokinetics was examined through a covariate analysis performed on data from 72 subjects: 48 white and 24 non-white. The apparent total body clearance and apparent volume of distribution were not affected by the race of the subjects.
Renal Impairment
Clearance of levofloxacin is substantially reduced and plasma elimination half-life is substantially prolonged in adult patients with impaired renal function (creatinine clearance < 50 mL/min), requiring dosage adjustment in such patients to avoid accumulation. Neither hemodialysis nor continuous ambulatory peritoneal dialysis (CAPD) is effective in removal of levofloxacin from the body, indicating that supplemental doses of levofloxacin are not required following hemodialysis or CAPD [see Dosage and Administration (2.3), Use in Specific Populations (8.6)].
Hepatic Impairment
Pharmacokinetic studies in hepatically impaired patients have not been conducted. Due to the limited extent of levofloxacin metabolism, the pharmacokinetics of levofloxacin are not expected to be affected by hepatic impairment [see Use in Specific Populations (8.7)].
Bacterial Infection
The pharmacokinetics of levofloxacin in patients with serious community-acquired bacterial infections are comparable to those observed in healthy subjects.
Drug-Drug Interactions
The potential for pharmacokinetic drug interactions between levofloxacin and antacids, warfarin, theophylline, cyclosporine, digoxin, probenecid, and cimetidine has been evaluated [see Drug Interactions (7)].
12.4 Microbiology
Mechanism of Action
Levofloxacin is the L-isomer of the racemate, ofloxacin, a quinolone antimicrobial agent. The antibacterial activity of ofloxacin resides primarily in the L-isomer. The mechanism of action of levofloxacin and other fluoroquinolone antimicrobials involves inhibition of bacterial topoisomerase IV and DNA gyrase (both of which are type II topoisomerases), enzymes required for DNA replication, transcription, repair and recombination.
Drug Resistance
Fluoroquinolone resistance can arise through mutations in defined regions of DNA gyrase or topoisomerase IV, termed the Quinolone-Resistance Determining Regions (QRDRs), or through altered efflux.
Fluoroquinolones, including levofloxacin, differ in chemical structure and mode of action from aminoglycosides, macrolides and β-lactam antibiotics, including penicillins. Fluoroquinolones may, therefore, be active against bacteria resistant to these antimicrobials.
Resistance to levofloxacin due to spontaneous mutation in vitro is a rare occurrence (range: 10-9 to 10-10). Although cross-resistance has been observed between levofloxacin and some other fluoroquinolones, some microorganisms resistant to other fluoroquinolones may be susceptible to levofloxacin.
Activity in vitro and in vivo
Levofloxacin has in vitro activity against a wide range of Gram-negative and Gram-positive microorganisms.
Levofloxacin is often bactericidal at concentrations equal to or slightly greater than inhibitory concentrations.
Levofloxacin has been shown to be active against most strains of the following microorganisms both in vitro and in clinical infections as described in Indications and Usage (1):
Aerobic Gram-Positive Microorganisms
Enterococcus faecalis (many strains are only moderately susceptible)
Staphylococcus aureus (methicillin-susceptible strains)
Staphylococcus epidermidis (methicillin-susceptible strains)
Streptococcus pneumoniae (including multi-drug resistant strains [MDRSP]1)
Streptococcus pyogenes
1 MDRSP (Multi-drug resistant Streptococcus pneumoniae) isolates are strains resistant to two or more of the following antibiotics: penicillin (MIC ≥2 mcg/mL), 2nd generation cephalosporins, e.g., cefuroxime; macrolides, tetracyclines and trimethoprim/sulfamethoxazole.
Aerobic Gram-Negative Microorganisms
Enterobacter cloacae
Escherichia coli
Haemophilus influenzae
Haemophilus parainfluenzae
Klebsiella pneumoniae
Legionella pneumophila
Moraxella catarrhalis
Proteus mirabilis
Pseudomonas aeruginosa2
Serratia marcescens
2 As with other drugs in this class some strains of Pseudomonas aeruginosa may develop resistance fairly rapidly during treatment with levofloxacin.
Other Microorganisms
Chlamydophila pneumoniae
Mycoplasma pneumoniae
Levofloxacin has been shown to be active against Bacillus anthracis both in vitro and by use of plasma levels as a surrogate marker in a rhesus monkey model for anthrax (post-exposure) [see Indications and Usage (1.13), Clinical Studies (14.9)].
The following in vitro data are available, but their clinical significance is unknown:
Levofloxacin exhibits in vitro minimum inhibitory concentrations (MIC values) of 2 mcg/mL or less against most (≥90%) strains of the following microorganisms; however, the safety and effectiveness of levofloxacin in treating clinical infections due to these microorganisms have not been established in adequate and well-controlled trials.
Aerobic Gram-Positive Microorganisms
Staphylococcus haemolyticus
β-hemolytic Streptococcus (Group C/F)
β-hemolytic Streptococcus (Group G)
Streptococcus agalactiae
Streptococcus milleri
Viridans group streptococci
Aerobic Gram-Negative Microorganisms
Acinetobacter baumannii
Acinetobacter lwoffii
Bordetella pertussis
Citrobacter koseri
Citrobacter freundii
Enterobacter aerogenes
Enterobacter sakazakii
Klebsiella oxytoca
Morganella morganii
Pantoea agglomerans
Proteus vulgaris
Providencia rettgeri
Providencia stuartii
Pseudomonas fluorescens
Anaerobic Gram-Positive Microorganisms
Clostridium perfringens
Susceptibility Tests
Susceptibility testing for levofloxacin should be performed, as it is the optimal predictor of activity.
• Dilution techniques:
Quantitative methods are used to determine antimicrobial minimal inhibitory concentrations (MIC values). These MIC values provide estimates of the susceptibility of bacteria to antimicrobial compounds. The MIC values should be determined using a standardized procedure. Standardized procedures are based on a dilution method1 (broth or agar) or equivalent with standardized inoculum concentrations and standardized concentrations of levofloxacin powder. The MIC values should be interpreted according to the criteria outlined in Table 9.
• Diffusion techniques:
Quantitative methods that require measurement of zone diameters also provide reproducible estimates of the susceptibility of bacteria to antimicrobial compounds. One such standardized procedure2 requires the use of standardized inoculum concentrations. This procedure uses paper disks impregnated with 5 mcg levofloxacin to test the susceptibility of microorganisms to levofloxacin.
Reports from the laboratory providing results of the standard single-disk susceptibility test with a 5 mcg levofloxacin disk should be interpreted according the criteria outlined in Table 9. Interpretation involves correlation of the diameter obtained in the disk test with the MIC for levofloxacin.
|
S = Susceptible, I = Intermediate, R = Resistant |
||||||
|
|
Minimum
Inhibitory
Concentrations ( mcg / mL ) |
Disk
Diffusion
( zone diameter in mm ) |
||||
|
Pathogen
|
S
|
I
|
R
|
S
|
I
|
R
|
|
Enterobacteriaceae
|
≤2 |
4 |
≥8 |
≥17 |
14-16 |
≤13 |
|
Enterococcus
faecalis
|
≤2 |
4 |
≥8 |
≥17 |
14-16 |
≤13 |
| Methicillin-susceptible Staphylococcus species |
≤2 |
4 |
≥8 |
≥17 |
14-16 |
≤13 |
|
Pseudomonas
aeruginosa
|
≤2 |
4 |
≥8 |
≥17 |
14-16 |
≤13 |
|
Haemophilus
influenzae
|
≤2 |
-- |
-- |
≥17 |
-- |
-- |
|
Haemophilus
parainfluenzae
|
≤2  |
-- |
-- |
≥17  |
-- |
-- |
|
Streptococcus
pneumoniae
|
≤2 |
4  |
≥8  |
≥17 |
14-16  |
≤13  |
|
Streptococcus
pyogenes
|
≤2 |
4 |
≥8 |
≥17 |
14-16 |
≤13 |
A report of Susceptible indicates that the pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of Intermediate indicates that the result should be considered equivocal, and, if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where a high dosage of drug can be used. This category also provides a buffer zone which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of Resistant indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
- Quality Control:
Standardized susceptibility test procedures require the use of laboratory control microorganisms to control the technical aspects of the laboratory procedures. For dilution technique, standard levofloxacin powder should give the MIC values provided in Table 10. For diffusion technique, the 5 mcg levofloxacin disk should provide zone diameters provided in Table 10.
|
* This quality control range is applicable to only H
.
influenzae ATCC 49247 tested by a broth microdilution procedure using Haemophilus Test Medium (HTM).1
|
|||
|
† This quality control range is applicable to only H
.
influenzae ATCC 49247 tested by a disk diffusion procedure using Haemophilus Test Medium (HTM).2
|
|||
|
‡ This quality control range is applicable to only S
.
pneumoniae ATCC 49619 tested by a broth microdilution procedure using cation-adjusted Mueller-Hinton broth with 2-5% lysed horse blood. |
|||
|
§ This quality control range is applicable to only S
.
pneumoniae ATCC 49619 tested by a disk diffusion procedure using Mueller-Hinton agar supplemented with 5% sheep blood and incubated in 5% CO2. |
|||
|
*
* Careful maintenance of this organism is required as the strain may lose its plasmid. |
|||
|
Microorganism
|
Microorganism
QC Number |
MIC
(
mcg
/
mL
)
|
Disk
Diffusion
( zone diameter in mm ) |
|
Enterococcus
faecalis
|
ATCC 29212 |
0.25 - 2 |
Not applicable |
|
Escherichia
coli
|
ATCC 25922 |
0.008 - 0.06 |
29 - 37 |
|
Escherichia
coli
*
*
|
ATCC 35218 |
0.015 - 0.06 |
Not applicable |
|
Haemophilus
influenzae
|
ATCC 49247 |
0.008 - 0.03*
|
32 - 40†
|
|
Pseudomonas
aeruginosa
|
ATCC 27853 |
0.5 - 4 |
19 - 26 |
|
Staphylococcus
aureus
|
ATCC 29213 |
0.06 - 0.5 |
Not applicable |
|
Staphylococcus
aureus
|
ATCC 25923 |
Not applicable |
25 - 30 |
|
Streptococcus
pneumoniae
|
ATCC 49619 |
0.5 - 2‡
|
20 - 25§
|
13. NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment Of Fertility
In a lifetime bioassay in rats, levofloxacin exhibited no carcinogenic potential following daily dietary administration for 2 years; the highest dose (100 mg/kg/day) was 1.4 times the highest recommended human dose (750 mg) based upon relative body surface area. Levofloxacin did not shorten the time to tumor development of UV-induced skin tumors in hairless albino (Skh-1) mice at any levofloxacin dose level and was therefore not photo-carcinogenic under conditions of this study. Dermal levofloxacin concentrations in the hairless mice ranged from 25 to 42 mcg/g at the highest levofloxacin dose level (300 mg/kg/day) used in the photo-carcinogenicity study. By comparison, dermal levofloxacin concentrations in human subjects receiving 750 mg of levofloxacin averaged approximately 11.8 mcg/g at Cmax.
Levofloxacin was not mutagenic in the following assays: Ames bacterial mutation assay (S. typhimurium and E. coli), CHO/HGPRT forward mutation assay, mouse micronucleus test, mouse dominant lethal test, rat unscheduled DNA synthesis assay, and the mouse sister chromatid exchange assay. It was positive in the in vitro chromosomal aberration (CHL cell line) and sister chromatid exchange (CHL/IU cell line) assays.
Levofloxacin caused no impairment of fertility or reproductive performance in rats at oral doses as high as 360 mg/kg/day, corresponding to 4.2 times the highest recommended human dose based upon relative body surface area and intravenous doses as high as 100 mg/kg/day, corresponding to 1.2 times the highest recommended human dose based upon relative body surface area.
13.2 Animal Toxicology And/Or Pharmacology
Levofloxacin and other quinolones have been shown to cause arthropathy in immature animals of most species tested [see Warnings and Precautions (5.10)]. In immature dogs (4-5 months old), oral doses of 10 mg/kg/day for 7 days and intravenous doses of 4 mg/kg/day for 14 days of levofloxacin resulted in arthropathic lesions. Administration at oral doses of 300 mg/kg/day for 7 days and intravenous doses of 60 mg/kg/day for 4 weeks produced arthropathy in juvenile rats. Three month old beagle dogs dosed orally with levofloxacin at 40 mg/kg/day exhibited clinically severe arthrotoxicity resulting in the termination of dosing at Day 8 of a 14-day dosing routine. Slight musculoskeletal clinical effects, in the absence of gross pathological or histopathological effects, resulted from the lowest dose level of 2.5 mg/kg/day (approximately 0.2-fold the pediatric dose based upon AUC comparisons). Synovitis and articular cartilage lesions were observed at the 10 and 40 mg/kg dose levels (approximately 0.7-fold and 2.4-fold the pediatric dose, respectively, based on AUC comparisons). Articular cartilage gross pathology and histopathology persisted to the end of the 18-week recovery period for those dogs from the 10 and 40 mg/kg/day dose levels.
When tested in a mouse ear swelling bioassay, levofloxacin exhibited phototoxicity similar in magnitude to ofloxacin, but less phototoxicity than other quinolones.
While crystalluria has been observed in some intravenous rat studies, urinary crystals are not formed in the bladder, being present only after micturition and are not associated with nephrotoxicity.
In mice, the CNS stimulatory effect of quinolones is enhanced by concomitant administration of non-steroidal anti-inflammatory drugs.
In dogs, levofloxacin administered at 6 mg/kg or higher by rapid intravenous injection produced hypotensive effects. These effects were considered to be related to histamine release.
In vitro and in vivo studies in animals indicate that levofloxacin is neither an enzyme inducer nor inhibitor in the human therapeutic plasma concentration range; therefore, no drug metabolizing enzyme-related interactions with other drugs or agents are anticipated.
14. CLINICAL STUDIES
14.1 Nosocomial Pneumonia
Adult patients with clinically and radiologically documented nosocomial pneumonia were enrolled in a multicenter, randomized, open-label study comparing intravenous levofloxacin (750 mg once daily) followed by oral levofloxacin (750 mg once daily) for a total of 7-15 days to intravenous imipenem/cilastatin (500-1000 mg every 6-8 hours daily) followed by oral ciprofloxacin (750 mg every 12 hours daily) for a total of 7-15 days. Levofloxacin-treated patients received an average of 7 days of intravenous therapy (range: 1-16 days); comparator-treated patients received an average of 8 days of intravenous therapy (range: 1-19 days).
Overall, in the clinically and microbiologically evaluable population, adjunctive therapy was empirically initiated at study entry in 56 of 93 (60.2%) patients in the levofloxacin arm and 53 of 94 (56.4%) patients in the comparator arm. The average duration of adjunctive therapy was 7 days in the levofloxacin arm and 7 days in the comparator. In clinically and microbiologically evaluable patients with documented Pseudomonas aeruginosa infection, 15 of 17 (88.2%) received ceftazidime (N=11) or piperacillin/tazobactam (N=4) in the levofloxacin arm and 16 of 17 (94.1%) received an aminoglycoside in the comparator arm. Overall, in clinically and microbiologically evaluable patients, vancomycin was added to the treatment regimen of 37 of 93 (39.8%) patients in the levofloxacin arm and 28 of 94 (29.8%) patients in the comparator arm for suspected methicillin-resistant S. aureus infection.
Clinical success rates in clinically and microbiologically evaluable patients at the posttherapy visit (primary study endpoint assessed on day 3-15 after completing therapy) were 58.1% for levofloxacin and 60.6% for comparator. The 95% Cl for the difference of response rates (levofloxacin minus comparator) was [-17.2, 12.0]. The microbiological eradication rates at the posttherapy visit were 66.7% for levofloxacin and 60.6% for comparator. The 95% Cl for the difference of eradication rates (levofloxacin minus comparator) was [-8.3, 20.3]. Clinical success and microbiological eradication rates by pathogen are detailed in Table 11.
|
* Methicillin-susceptible S
.
aureus
|
||||
|
† See above text for use of combination therapy |
||||
|
‡ The observed differences in rates for the clinical and microbiological outcomes may reflect other factors that were not accounted for in the study |
||||
|
Pathogen
|
N
|
Levofloxacin
No
.
(%)
of
Patients
Microbiologic
/
Clinical Outcomes |
N
|
Imipenem
/
Cilastatin
No . (%) of Patients Microbiologic / Clinical Outcomes |
| MSSA* |
21 |
14 (66.7)/13 (61.9) |
19 |
13 (68.4)/15 (78.9) |
|
P
.
aeruginosa
†
|
17 |
10 (58.8)/11 (64.7) |
17 |
5 (29.4)/7 (41.2) |
|
S
.
marcescens
|
11 |
9 (81.8)/7 (63.6) |
7 |
2 (28.6)/3 (42.9) |
|
E
.
coli
|
12 |
10 (83.3)/7 (58.3) |
11 |
7 (63.6 )/8 (72.7) |
|
K
.
pneumoniae
‡
|
11 |
9 (81.8)/5 (45.5) |
7 |
6 (85.7)/3 (42.9) |
|
H
.
influenzae
|
16 |
13 (81.3)/10 (62.5) |
15 |
14 (93.3)/11 (73.3) |
|
S
.
pneumoniae
|
4 |
3 (75.0)/3 (75.0) |
7 |
5 (71.4)/4 (57.1) |
14.2 Community-Acquired Pneumonia: 7-14 day Treatment Regimen
Adult inpatients and outpatients with a diagnosis of community-acquired bacterial pneumonia were evaluated in 2 pivotal clinical studies. In the first study, 590 patients were enrolled in a prospective, multi-center, unblinded randomized trial comparing levofloxacin 500 mg once daily orally or intravenously for 7 to 14 days to ceftriaxone 1 to 2 grams intravenously once or in equally divided doses twice daily followed by cefuroxime axetil 500 mg orally twice daily for a total of 7 to 14 days. Patients assigned to treatment with the control regimen were allowed to receive erythromycin (or doxycycline if intolerant of erythromycin) if an infection due to atypical pathogens was suspected or proven. Clinical and microbiologic evaluations were performed during treatment, 5 to 7 days posttherapy, and 3 to 4 weeks posttherapy. Clinical success (cure plus improvement) with levofloxacin at 5 to 7 days posttherapy, the primary efficacy variable in this study, was superior (95%) to the control group (83%). The 95% Cl for the difference of response rates (levofloxacin minus comparator) was [-6, 19]. In the second study, 264 patients were enrolled in a prospective, multi-center, non-comparative trial of 500 mg levofloxacin administered orally or intravenously once daily for 7 to 14 days. Clinical success for clinically evaluable patients was 93%. For both studies, the clinical success rate in patients with atypical pneumonia due to Chlamydophila pneumoniae, Mycoplasma pneumoniae, and Legionella pneumophila were 96%, 96%, and 70%, respectively. Microbiologic eradication rates across both studies are presented in Table 12.
|
Pathogen
|
No
.
Pathogen
|
Microbiologic
Eradication
Rate
(%)
|
|
H
.
influenzae
|
55 |
98 |
|
S
.
pneumoniae
|
83 |
95 |
|
S
.
aureus
|
17 |
88 |
|
M
.
catarrhalis
|
18 |
94 |
|
H
.
parainfluenzae
|
19 |
95 |
|
K
.
pneumoniae
|
10 |
100.0 |
Community-Acquired Pneumonia Due to Multi-Drug Resistant Streptococcus pneumoniae
Levofloxacin was effective for the treatment of community-acquired pneumonia caused by multi-drug resistant Streptococcus pneumoniae (MDRSP). MDRSP isolates are strains resistant to two or more of the following antibacterials: penicillin (MIC ≥2 mcg/mL), 2nd generation cephalosporins (e.g., cefuroxime, macrolides, tetracyclines and trimethoprim/sulfamethoxazole). Of 40 microbiologically evaluable patients with MDRSP isolates, 38 patients (95.0%) achieved clinical and bacteriologic success at post-therapy. The clinical and bacterial success rates are shown in Table 13.
|
* One patient had a respiratory isolate that was resistant to tetracycline, cefuroxime, macrolides and TMP/SMX and intermediate to penicillin and a blood isolate that was intermediate to penicillin and cefuroxime and resistant to the other classes. The patient is included in the database based on respiratory isolate.
|
||||
|
† n=the number of microbiologically evaluable patients who were clinical successes; N=number of microbiologically evaluable patients in the designated resistance group. |
||||
|
‡ n=the number of MDRSP isolates eradicated or presumed eradicated in microbiologically evaluable patients; N=number of MDRSP isolates in a designated resistance group. |
||||
|
|
||||
|
Screening
Susceptibility
|
Clinical
Success
|
Bacteriological
Success
*
|
||
|
|
n
/
N
†
|
%
|
n
/
N
‡
|
%
|
|
Penicillin
-
resistant
|
16/17 |
94.1 |
16/17 |
94.1 |
|
2nd
generation
Cephalosporin resistant |
31/32 |
96.9 |
31/32 |
96.9 |
|
Macrolide
-
resistant
|
28/29 |
96.6 |
28/29 |
96.6 |
|
Trimethoprim
/
Sulfamethoxazole resistant |
17/19 |
89.5 |
17/19 |
89.5 |
|
Tetracycline
-
resistant
|
12/12 |
100 |
12/12 |
100 |
14.3 Community-Acquired Pneumonia: 5-Day Treatment Regimen
To evaluate the safety and efficacy of higher dose and shorter course of levofloxacin, 528 outpatient and hospitalized adults with clinically and radiologically determined mild to severe community-acquired pneumonia were evaluated in a double-blind, randomized, prospective, multicenter study comparing levofloxacin 750 mg, IV or orally, every day for five days or levofloxacin 500 mg IV or orally, every day for 10 days.
Clinical success rates (cure plus improvement) in the clinically evaluable population were 90.9% in the levofloxacin 750 mg group and 91.1% in the levofloxacin 500 mg group. The 95% Cl for the difference of response rates (Levofloxacin 750 minus levofloxacin 500) was [-5.9, 5.4]. In the clinically evaluable population (31-38 days after enrollment) pneumonia was observed in 7 out of 151 patients in the levofloxacin 750 mg group and 2 out of 147 patients in the levofloxacin 500 mg group. Given the small numbers observed, the significance of this finding cannot be determined statistically. The microbiological efficacy of the 5-day regimen was documented for infections listed in Table 15.
| Penicillin susceptible S
.
pneumoniae
|
19/20 |
|
Haemophilus
influenzae
|
12/12 |
|
Haemophilus
parainfluenzae
|
10/10 |
|
Mycoplasma
pneumoniae
|
26/27 |
|
Chlamydophila
pneumoniae
|
13/15 |
14.4 Acute Bacterial Sinusitis: 5-day and 10-14 day Treatment Regimens
Levofloxacin is approved for the treatment of acute bacterial sinusitis (ABS) using either 750 mg by mouth x 5 days or 500 mg by mouth once daily x 10-14 days. To evaluate the safety and efficacy of a high dose short course of levofloxacin, 780 outpatient adults with clinically and radiologically determined acute bacterial sinusitis were evaluated in a double-blind, randomized, prospective, multicenter study comparing levofloxacin 750 mg by mouth once daily for five days to 500 mg by mouth once daily for 10 days.
Clinical success rates (defined as complete or partial resolution of the pre-treatment signs and symptoms of ABS to such an extent that no further antibiotic treatment was deemed necessary) in the microbiologically evaluable population were 91.4% (139/152) in the levofloxacin 750 mg group and 88.6% (132/149) in the levofloxacin 500 mg group at the test-of-cure (TOC) visit (95% Cl [-4.2, 10.0] for levofloxacin 750 mg minus levofloxacin 500 mg).
Rates of clinical success by pathogen in the microbiologically evaluable population who had specimens obtained by antral tap at study entry showed comparable results for the five- and ten-day regimens at the test-of-cure visit 22 days post treatment.
|
* Note: Forty percent of the subjects in this trial had specimens obtained by sinus endoscopy. The efficacy data for subjects whose specimen was obtained endoscopically were comparable to those presented in the above table. |
||
|
Pathogen
|
Levofloxacin
750 mg x 5 days |
Levofloxacin
500 mg x 10 days |
|
Streptococcus
pneumoniae* |
25/27(92.6%) |
26/27 (96.3%) |
|
Haemophilus
influenzae* |
19/21 (90.5%) |
25/27 (92.6%) |
|
Moraxella
catarrhalis* |
10/11 (90.9%) |
13/13 (100%) |
14.5 Complicated Skin and Skin Structure Infections
Three hundred ninety-nine patients were enrolled in an open-label, randomized, comparative study for complicated skin and skin structure infections. The patients were randomized to receive either levofloxacin 750 mg once daily (IV followed by oral), or an approved comparator for a median of 10 ± 4.7 days. As is expected in complicated skin and skin structure infections, surgical procedures were performed in the levofloxacin and comparator groups. Surgery (incision and drainage or debridement) was performed on 45% of the levofloxacin-treated patients and 44% of the comparator-treated patients, either shortly before or during antibiotic treatment and formed an integral part of therapy for this indication.
Among those who could be evaluated clinically 2-5 days after completion of study drug, overall success rates (improved or cured) were 116/138 (84.1%) for patients treated with levofloxacin and 106/132 (80.3%) for patients treated with the comparator.
Success rates varied with the type of diagnosis ranging from 68% in patients with infected ulcers to 90% in patients with infected wounds and abscesses. These rates were equivalent to those seen with comparator drugs.
14.6 Chronic Bacterial Prostatitis
Adult patients with a clinical diagnosis of prostatitis and microbiological culture results from urine sample collected after prostatic massage (VB3) or expressed prostatic secretion (EPS) specimens obtained via the Meares-Stamey procedure were enrolled in a multicenter, randomized, double-blind study comparing oral levofloxacin 500 mg, once daily for a total of 28 days to oral ciprofloxacin 500 mg, twice daily for a total of 28 days. The primary efficacy endpoint was microbiologic efficacy in microbiologically evaluable patients. A total of 136 and 125 microbiologically evaluable patients were enrolled in the levofloxacin and ciprofloxacin groups, respectively. The microbiologic eradication rate by patient infection at 5-18 days after completion of therapy was 75.0% in the levofloxacin group and 76.8% in the ciprofloxacin group (95% Cl [-12.58, 8.98] for levofloxacin minus ciprofloxacin). The overall eradication rates for pathogens of interest are presented in Table 17.
|
* Eradication rates shown are for patients who had a sole pathogen only; mixed cultures were excluded. |
||||
|
|
||||
|
|
Levofloxacin
(
N
=
136
)
|
Ciprofloxacin
(
N
=
125
)
|
||
|
Pathogen
|
N
|
Eradication
|
N
|
Eradication
|
|
E
.
coli
|
15 |
14 (93.3%) |
11 |
9 (81.8%) |
|
E
.
faecalis
|
54 |
39 (72.2%) |
44 |
33 (75.0%) |
|
S
.
epidermidis
*
|
11 |
9 (81.8%) |
14 |
11 (78.6%) |
14.7 Complicated Urinary Tract Infections and Acute Pyelonephritis: 5-day Treatment Regimen
To evaluate the safety and efficacy of the higher dose and shorter course of levofloxacin, 1109 patients with cUTI and AP were enrolled in a randomized, double-blind, multicenter clinical trial conducted in the US from November 2004 to April 2006 comparing levofloxacin 750 mg IV or orally once daily for 5 days (546 patients) with ciprofloxacin 400 mg IV or 500 mg orally twice daily for 10 days (563 patients). Patients with AP complicated by underlying renal diseases or conditions such as complete obstruction, surgery, transplantation, concurrent infection or congenital malformation were excluded. Efficacy was measured by bacteriologic eradication of the baseline organism(s) at the post-therapy visit in patients with a pathogen identified at baseline. The post-therapy (test-of-cure) visit occurred 10 to 14 days after the last active dose of levofloxacin and 5 to 9 days after the last dose of active ciprofloxacin.
The bacteriologic cure rates overall for levofloxacin and control at the test-of-cure (TOC) visit for the group of all patients with a documented pathogen at baseline (modified intent to treat or mITT) and the group of patients in the mITT population who closely followed the protocol (Microbiologically Evaluable) are summarized in Table 18.
|
* The mITT population included patients who received study medication and who had a positive (≥ 105 CFU/mL) urine culture with no more than 2 uropathogens at baseline. Patients with missing response were counted as failures in this analysis. |
|||||
|
†
The Microbiologically Evaluable population included patients with a confirmed diagnosis of cUTI or AP, a causative organism(s) at baseline present at ≥105 CFU/mL, a valid test-of-cure urine culture, no pathogen isolated from blood resistant to study drug, no premature discontinuation or loss to follow-up, and compliance with treatment (among other criteria). |
|||||
|
|
Levofloxacin
750 mg orally or IV once daily for 5 days |
Ciprofloxacin
400 mg IV/500 mg orally twice daily for 10 days |
Overall
Difference [ 95 % Cl ] |
||
|
|
n/N |
% |
n/N |
% |
Levofloxacin - Ciprofloxacin |
|
mITT
Population
*
|
|||||
| Overall (cUTI or AP)
|
252/333
|
75.7 |
239/318 |
75.2 |
0.5 (-6.1, 7.1) |
| cUTI
|
168/230
|
73.0 |
157/213 |
73.7 |
|
| AP |
84/103
|
81.6 |
82/105 |
78.1 |
|
|
Microbiologically
Evaluable
Population
†
|
|||||
| Overall (cUTI or AP)
|
228/265
|
86.0 |
215/241 |
89.2 |
-3.2 [-8.9, 2.5]
|
| cUTI
|
154/185
|
83.2 |
144/165 |
87.3 |
|
| AP |
74/80
|
92.5 |
71/76 |
93.4 |
|
14.8 Complicated Urinary Tract Infections and Acute Pyelonephritis: 10-day Treatment Regimen
To evaluate the safety and efficacy of the 250 mg dose, 10 day regimen of levofloxacin, 567 patients with uncomplicated UTI, mild-to-moderate cUTI, and mild-to-moderate AP were enrolled in a randomized, double-blind, multicenter clinical trial conducted in the US from June 1993 to January 1995 comparing levofloxacin 250 orally once daily for 10 days (285 patients) with ciprofloxacin 500 mg orally twice daily for 10 days (282 patients). Patients with a resistant pathogen, recurrent UTI, women over age 55 years, and with an indwelling catheter were initially excluded, prior to protocol amendment which took place after 30% of enrollment. Microbiological efficacy was measured by bacteriologic eradication of the baseline organism(s) at 1-12 days posttherapy in patients with a pathogen identified at baseline.
The bacteriologic cure rates overall for levofloxacin and control at the test-of-cure (TOC) visit for the group of all patients with a documented pathogen at baseline (modified intent to treat or mITT) and the group of patients in the mITT population who closely followed the protocol (Microbiologically Evaluable) are summarized in Table 20.
|
* 1-9 days posttherapy for 30% of subjects enrolled prior to a protocol amendment; 5-12 days posttherapy for 70% of subjects. |
||||
|
† The mITT population included patients who had a pathogen isolated at baseline. Patients with missing response were counted as failures in this analysis. |
||||
|
‡ The Microbiologically Evaluable population included mITT patients who met protocol-specified evaluability criteria. |
||||
|
|
Levofloxacin
250 mg once daily for 10 days |
Ciprofloxacin
500 mg twice daily for 10 days |
||
|
|
n/N
|
% |
n/N
|
% |
|
mITT
Population
†
|
174/209 |
83.3 |
184/219 |
84.0 |
|
Microbiologically
Evaluable Population ‡ |
164/177 |
92.7 |
159/171 |
93.0 |
14.9 Inhalational Anthrax (Post-Exposure)
The effectiveness of levofloxacin for this indication is based on plasma concentrations achieved in humans, a surrogate endpoint reasonably likely to predict clinical benefit. Levofloxacin has not been tested in humans for the post-exposure prevention of inhalation anthrax. The mean plasma concentrations of levofloxacin associated with a statistically significant improvement in survival over placebo in the rhesus monkey model of inhalational anthrax are reached or exceeded in adult and pediatric patients receiving the recommended oral and intravenous dosage regimens [see Indications and Usage (1.13); Dosage and Administration (2.1, 2.2)].
Levofloxacin pharmacokinetics have been evaluated in adult and pediatric patients. The mean (± SD) steady state peak plasma concentration in human adults receiving 500 mg orally or intravenously once daily is 5.7 ± 1.4 and 6.4 ± 0.8 mcg/mL, respectively; and the corresponding total plasma exposure (AUC0-24) is 47.5 ± 6.7 and 54.6 ± 11.1 mcg.h/mL, respectively. The predicted steady-state pharmacokinetic parameters in pediatric patients ranging in age from 6 months to 17 years receiving 8 mg/kg orally every 12 hours (not to exceed 250 mg per dose) were calculated to be comparable to those observed in adults receiving 500 mg orally once daily [see Clinical Pharmacology (12.3)].
In adults, the safety of levofloxacin for treatment durations of up to 28 days is well characterized. However, information pertaining to extended use at 500 mg daily up to 60 days is limited. Prolonged levofloxacin therapy in adults should only be used when the benefit outweighs the risk.
In pediatric patients, the safety of levofloxacin for treatment durations of more than 14 days has not been studied. An increased incidence of musculoskeletal adverse events (arthralgia, arthritis, tendinopathy, gait abnormality) compared to controls has been observed in clinical studies with treatment duration of up to 14 days. Long-term safety data, including effects on cartilage, following the administration of levofloxacin to pediatric patients is limited [see Warnings and Precautions (5.10), Use in Specific Populations (8.4)].
A placebo-controlled animal study in rhesus monkeys exposed to an inhaled mean dose of 49 LD50 (~2.7 X 106) spores (range 17 - 118 LD50) of B. anthracis (Ames strain) was conducted. The minimal inhibitory concentration (MIC) of levofloxacin for the anthrax strain used in this study was 0.125 mcg/mL. In the animals studied, mean plasma concentrations of levofloxacin achieved at expected Tmax (1 hour post-dose) following oral dosing to steady state ranged from 2.79 to 4.87 mcg/mL. Steady state trough concentrations at 24 hours post-dose ranged from 0.107 to 0.164 mcg/mL. Mean (SD) steady state AUC0-24 was 33.4 ± 3.2 mcg.h/mL (range 30.4 to 36.0 mcg.h/mL). Mortality due to anthrax for animals that received a 30 day regimen of oral levofloxacin beginning 24 hrs post exposure was significantly lower (1/10), compared to the placebo group (9/10) [P=0.0011, 2-sided Fisher’s Exact Test]. The one levofloxacin treated animal that died of anthrax did so following the 30-day drug administration period.
15. REFERENCES
- Clinical and Laboratory Standards Institute. Methods for Dilution Antimicrobial Susceptibility Tests for Bacteria That Grow Aerobically. Approved Standard – Eighth Edition. Clinical and Laboratory Standards Institute document M7-A8, Vol. 29, No. 2, CLSI, Wayne, PA, January 2009.
- Clinical and Laboratory Standards Institute. Performance Standards for Antimicrobial Disk Susceptibility Tests. Approved Standard – Tenth Edition. Clinical and Laboratory Standards Institute document M2-A10, Vol. 29, No. 1, CLSI, Wayne, PA, January 2009.
16. HOW SUPPLIED/STORAGE AND HANDLING
16.1 Levofloxacin Tablets
Levofloxacin Tablets are supplied as 250, 500, and 750 mg capsule-shaped, coated tablets. Levofloxacin tablets are packaged in bottles and in unit-dose blister strips in the following configurations:
Levofloxacin tablets 250 mg are light pink colored capsule-shaped film-coated tablets debossed with "250" on one side and "1082" on the other side.
Bottles of 50 NDC 13668-082-50
Bottles of 100 NDC 13668-082-01
Bottles of 500 NDC 13668-082-05
100 Unit dose tablets NDC 13668-082-74
Levofloxacin tablets 500 mg are brick red colored capsule-shaped film-coated tablets debossed with "83" on one side and plain on the other side.
Bottles of 50 NDC 13668-083-50
Bottles of 100 NDC 13668-083-01
Bottles of 500 NDC 13668-083-05
100 Unit dose tablets NDC 13668-083-74
Levofloxacin tablets 750 mg are white to off-white colored capsule-shaped film-coated tablets debossed with "750" on one side and "1084" on the other side.
Bottles of 20 NDC 13668-084-21
Bottles of 50 NDC 13668-084-50
Bottles of 100 NDC 13668-084-01
Bottles of 500 NDC 13668-084-05
100 Unit dose tablets NDC 13668-084-74
Levofloxacin tablets should be stored at 20° to 25°C (68° to 77°); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Dispense in tight, light-resistant container with a child-resistant closure.
17. PATIENT COUNSELING INFORMATION
See FDA-Approved Medication Guide (17.5)
17.1 Antibacterial Resistance
Antibacterial drugs including levofloxacin tablets should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When levofloxacin tablets are prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by levofloxacin tablets or other antibacterial drugs in the future.
17.2 Administration with Food, Fluids, and Concomitant Medications
Patients should be informed that levofloxacin tablets may be taken with or without food. The tablet should be taken at the same time each day.
Patients should drink fluids liberally while taking levofloxacin tablets to avoid formation of a highly concentrated urine and crystal formation in the urine.
Antacids containing magnesium, or aluminum, as well as sucralfate, metal cations such as iron, and multivitamin preparations with zinc or didanosine should be taken at least two hours before or two hours after oral levofloxacin tablet administration.
17.3 Serious and Potentially Serious Side Effects
Patients should be informed of the following serious adverse reactions that have been associated with levofloxacin or other fluoroquinolone use:
- Tendon Disorders: Patients should contact their healthcare provider if they experience pain, swelling, or inflammation of a tendon, or weakness or inability to use one of their joints; rest and refrain from exercise; and discontinue levofloxacin treatment. The risk of severe tendon disorders with fluoroquinolones is higher in older patients usually over 60 years of age, in patients taking corticosteroid drugs, and in patients with kidney, heart or lung transplants.
- Exacerbation of Myasthenia Gravis: Patients should inform their physician of any history of myasthenia gravis. Patients should notify their physician if they experience any symptoms of muscle weakness, including respiratory difficulties.
- Hypersensitivity Reactions: Patients should be informed that levofloxacin can cause hypersensitivity reactions, even following the first dose. Patients should discontinue the drug at the first sign of a skin rash, hives or other skin reactions, a rapid heartbeat, difficulty in swallowing or breathing, any swelling suggesting angioedema (e.g., swelling of the lips, tongue, face, tightness of the throat, hoarseness), or other symptoms of an allergic reaction.
- Hepatotoxicity: Severe hepatotoxicity (including acute hepatitis and fatal events) has been reported in patients taking levofloxacin. Patients should inform their physician and be instructed to discontinue levofloxacin treatment immediately if they experience any signs or symptoms of liver injury including: loss of appetite, nausea, vomiting, fever, weakness, tiredness, right upper quadrant tenderness, itching, yellowing of the skin and eyes, light colored bowel movements or dark colored urine.
- Convulsions: Convulsions have been reported in patients taking fluoroquinolones, including levofloxacin tablets. Patients should notify their physician before taking this drug if they have a history of convulsions.
- Neurologic Adverse Effects (e.g., dizziness, lightheadedness): Patients should know how they react to levofloxacin tablets before they operate an automobile or machinery or engage in other activities requiring mental alertness and coordination.
- Diarrhea: Diarrhea is a common problem caused by antibiotics which usually ends when the antibiotic is discontinued. Sometimes after starting treatment with antibiotics, patients can develop watery and bloody stools (with or without stomach cramps and fever) even as late as two or more months after having taken the last dose of the antibiotic. If this occurs, patients should contact their physician as soon as possible.
- Peripheral Neuropathies: If symptoms of peripheral neuropathy including pain, burning, tingling, numbness, and/or weakness develop, patients should discontinue treatment and contact their physician.
- Prolongation of the QT Interval: Patients should inform their physician of any personal or family history of QT prolongation or proarrhythmic conditions such as hypokalemia, bradycardia, or recent myocardial ischemia; if they are taking any class IA (quinidine, procainamide), or class III (amiodarone, sotalol) antiarrhythmic agents. Patients should notify their physicians if they have any symptoms of prolongation of the QT interval, including prolonged heart palpitations or a loss of consciousness.
- Musculoskeletal Disorders in Pediatric Patients: Parents should inform their child's physician if their child has a history of joint-related problems before taking this drug. Parents of pediatric patients should also notify their child's physician of any tendon or joint-related problems that occur during or following levofloxacin therapy [see Warnings and Precautions (5.10) and Use in Specific Populations (8.4)].
- Photosensitivity/Phototoxicity: Patients should be advised that photosensitivity/phototoxicity has been reported in patients receiving fluoroquinolone antibiotics. Patients should minimize or avoid exposure to natural or artificial sunlight (tanning beds or UVA/B treatment) while taking fluoroquinolones. If patients need to be outdoors when taking fluoroquinolones, they should wear loose-fitting clothes that protect skin from sun exposure and discuss other sun protection measures with their physician. If a sunburn like reaction or skin eruption occurs, patients should contact their physician.
17.4 Drug Interactions with Insulin, Oral Hypoglycemic Agents, and Warfarin
Patients should be informed that if they are diabetic and are being treated with insulin or an oral hypoglycemic agent and a hypoglycemic reaction occurs, they should discontinue levofloxacin and consult a physician.
Patients should be informed that concurrent administration of warfarin and levofloxacin has been associated with increases of the International Normalized Ratio (INR) or prothrombin time and clinical episodes of bleeding. Patients should notify their physician if they are taking warfarin, be monitored for evidence of bleeding, and also have their anticoagulation tests closely monitored while taking warfarin concomitantly.

17.5 FDA-Approved Medication Guide
MEDICATION GUIDE
Levofloxacin Tablets
Rx Only
250 mg Tablets, 500 mg Tablets, and 750 mg Tablets
Read the Medication Guide that comes with levofloxacin tablets before you start taking them and each time you get a refill. There may be new information. This Medication Guide does not take the place of talking to your healthcare provider about your medical condition or your treatment.
What is the most important information I should know about levofloxacin tablets?
Levofloxacin belongs to a class of antibiotics called fluoroquinolones. Levofloxacin tablets can cause side effects that may be serious or even cause death. If you get any of the following serious side effects, get medical help right away. Talk with your healthcare provider about whether you should continue to take levofloxacin tablets.
- Tendon rupture or swelling of the tendon (tendinitis).
- Tendons are tough cords of tissue that connect muscles to bones.
- Pain, swelling, tears, and inflammation of tendons including the back of the ankle (Achilles), shoulder, hand, or other tendon sites can happen in people of all ages who take fluoroquinolone antibiotics, including levofloxacin tablets. The risk of getting tendon problems is higher if you:
- are over 60 years of age
- are taking steroids (corticosteroids)
- have had a kidney, heart, or lung transplant.
- Swelling of the tendon (tendinitis) and tendon rupture (breakage) have also happened in patients who take fluoroquinolones who do not have the above risk factors.
- Other reasons for tendon ruptures can include:
- physical activity or exercise
- kidney failure
- tendon problems in the past, such as in people with rheumatoid arthritis (RA).
- Call your healthcare provider right away at the first sign of tendon pain, swelling or inflammation. Stop taking levofloxacin tablets until tendinitis or tendon rupture has been ruled out by your healthcare provider. Avoid exercise and using the affected area. The most common area of pain and swelling is the Achilles tendon at the back of your ankle. This can also happen with other tendons. Talk to your healthcare provider about the risk of tendon rupture with continued use of levofloxacin tablets. You may need a different antibiotic that is not a fluoroquinolone to treat your infection.
- Tendon rupture can happen while you are taking or after you have finished taking levofloxacin tablets. Tendon ruptures have happened up to several months after patients have finished taking their fluoroquinolone.
- Get medical help right away if you get any of the following signs or symptoms of a tendon rupture:
- hear or feel a snap or pop in a tendon area
- bruising right after an injury in a tendon area
- unable to move the affected area or bear weight
- Worsening of myasthenia gravis (a disease that causes muscle weakness).
PACKAGE LABEL.PRINCIPAL DISPLAY PANEL
Levofloxacin Tablets 250 mg, 500s count

Levofloxacin Tablets 500 mg, 500s count

Levofloxacin Tablets 750 mg, 500s count

levofloxacinlevofloxacin TABLET
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||